Angela Reiersen, MD, MPE
@AngelaReiersen
Followers
5,750
Following
5,913
Media
268
Statuses
6,672
Associate Professor of Psychiatry @WUSTL ; Opinions are my own; Tweets are not medical advice. Say my name:
St Louis, MO
Joined October 2020
Don't wanna be here?
Send us removal request.
Explore trending content on Musk Viewer
#母の日
• 337969 Tweets
#นาฏราชครั้งที่15
• 309964 Tweets
WIN AT NATARAJA AWARDS
• 119280 Tweets
Feliz Dia
• 117976 Tweets
テンハッピーローズ
• 109104 Tweets
Mães
• 84346 Tweets
#光る君へ
• 71957 Tweets
カーネーション
• 54573 Tweets
MC NUNEW EP1
• 49618 Tweets
Cibeles
• 44500 Tweets
#やまラスト
• 37877 Tweets
新ビジュ
• 35582 Tweets
DONBELLE BOX OFFICE LEGACY
• 31905 Tweets
Ohm X Nataraja Awards
• 17094 Tweets
#光る君ヘ
• 16011 Tweets
GENCelebrate Music With BINI
• 12262 Tweets
清少納言
• 10366 Tweets
Last Seen Profiles
Ontario becomes the first province to list fluvoxamine as a COVID-19 treatment to consider via
@CTVNews
32
212
629
Just published a new paper with
@Bradley_A_Fritz
,
@EricLenze2
,
@farid__jalali
, and
@HoertelN
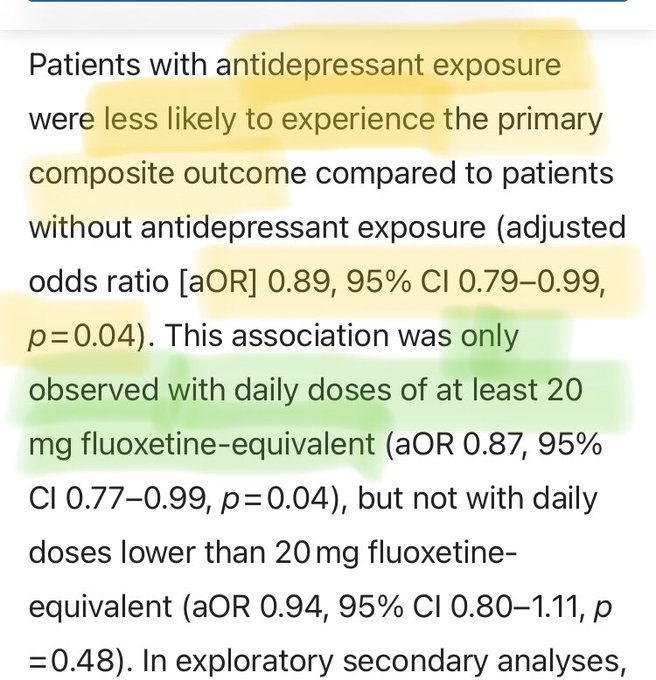
. It seems that any of several antidepressants can have protective effects against severe COVID outcomes (ER visits, hospitalizations).
26
131
444
Just watched this. I have not been totally convinced that ivermectin works as well as some people think it does, but there is enough evidence for it and low enough risk of harm from the drug, that this should be taken seriously.
H-Hour: 0900, D-Day: 6/1/21
Tuesday, 9am Pacific, I will be talking live in the DarkHorse studio with
@PierreKory
of FLCCC /
@Covid19Critical
on the pandemic, the care of COVID-19 patients and the multidimensional campaign against Ivermectin. Buckle up...
241
1K
3K
27
44
192
There is good evidence for treating COVID early with monoclonal antibodies and fluvoxamine. It is important to get the word out, so people who become ill will know they can talk to their doctors about treatment options.
@firasd
I don't think it's dishonest to say that there are innovative treatment options, I think it's just true! And while monoclonal antibodies in particular are highly effective, uptake isn't very high, which is part of why Covid is still a problem.
2
1
20
13
59
169
Fluvoxamine EUA application has been submitted.
#IDTwitter
we submitted EUA Application for
#Fluvoxamine
for
#COVID19
to
@US_FDA
with the assistance of
@EricLenze2
@AngelaReiersen
@drklausner
@ShohamTxID
, and Ed Mills
If you want to sign a letter of support
(names are not public & will be reviewed)
14
43
139
12
37
144
Our full paper on possible mechanisms of fluvoxamine in treating COVID19 has now been published in
@FrontiersIn
Pharmacology.
16
53
140
Case reports on 2 COVID19 patients showing signs of serotonin excess & improving with cyproheptadine. If this is caused by platelet hyperactivation, an SSRI given early in the course of COVID19 could potentially prevent this.
@farid__jalali
Check out my published case reports on 2 patients with what appears to be an unprovoked serotonin-like syndrome in
#covid19
#medtwitter
please share
@TelehealthBot
0
22
48
10
35
129
This situation seem pretty bad, but there is a good COVID19 outpatient treatment option that many people are ignoring or have not heard about: FLUVOXAMINE.
2. Lack of Rx options. At least one of our mabs not effective vs omicron due to SGTF mutations and as
@EricTopol
points out in his new opinion piece we don’t have paxlovid in quantity
17
40
284
8
38
124
@Covid19Crusher
Increase in melatonin level may be one reason for fluvoxamine’s apparent benefit. Maybe they are even better given together.
4
34
106
@amandalhu
Some pro-vax people are also anti-early-treatment for some reason. Sometimes when I post about COVID treatment research findings, some pro-vax people pop out and say they’d prefer to just get vaxxed. Getting vaxxed does not 100% prevent COVID. We need treatments too.
8
17
93
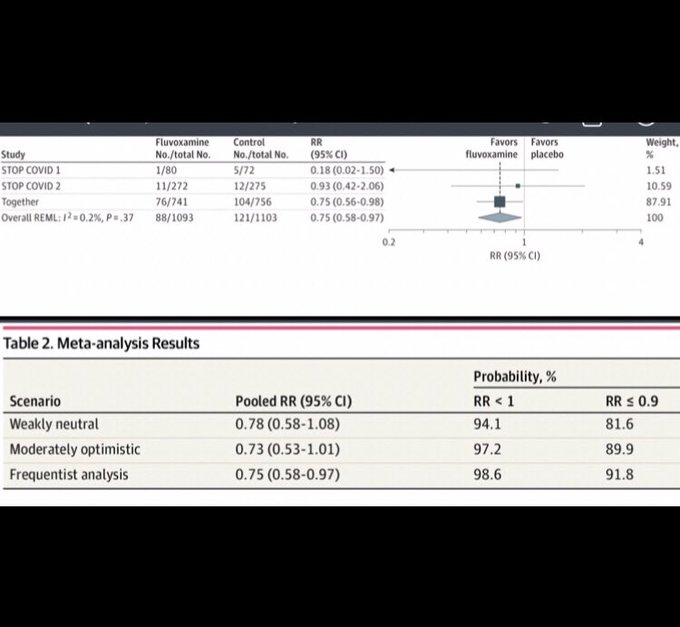
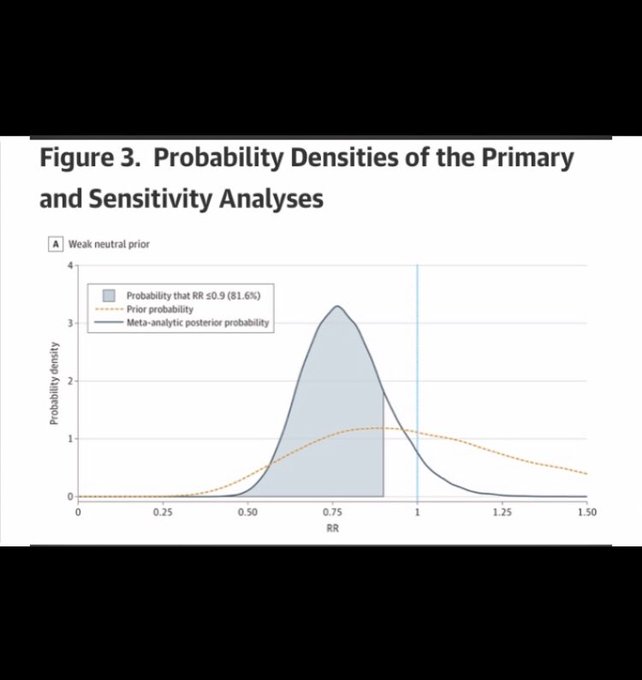
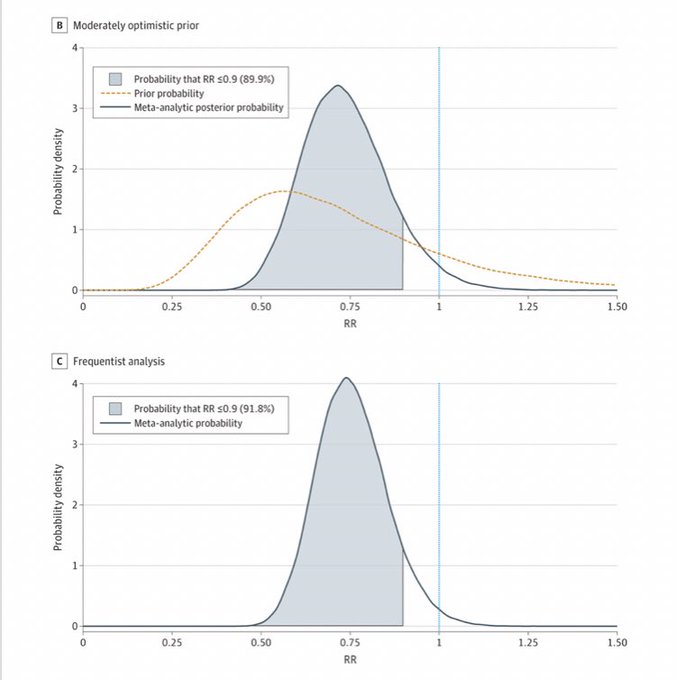
Meta-analysis has been published: Fluvoxamine for Outpatient Management of COVID-19 to Prevent Hospitalization via
@JAMANetworkOpen
part of
@JAMANetwork
3
23
90
Thanks to Sharyn Alfonsi and the
@60Minutes
@CBS
team for this excellent story about our fluvoxamine studies.
@EricLenze2
@WUSTLmed
#COVID19
#60Minutes
#fluvoxamine
COVID-19 research points to repurposed drugs
11
29
88
It’s great that Paxlovid will be available, but not everyone with COVID will be able to get it, at least not at first. Fluvoxamine can be prescribed off-label for outpatients with acute COVID NOW.
9
21
86
This is an important study by
@farid__jalali
and colleagues on platelets & serotonin in COVID19.
1
39
85
@EricTopol
@NatureMicrobiol
I'd be very interested in getting a nasal vaccine against this virus, especially if a nasal vaccine might be less likely than other existing vaccines to trigger autoimmune/inflammatory-related long COVID symptom flares.
4
6
86
I agree with this tweet by
@farid__jalali
. We need BOTH vaccines AND early treatment options for COVID.
19
18
82
So, if Paxlovid only “pauses” viral replication, and the course of illness can just continue on once Paxlovid is stopped, maybe it would work better if combined with something else that has a different mechanism.
@AngelaReiersen
@DrSyedHaider2
@drbeen_medical
@ichudov
@Aguirre1Gustavo
@DarrellMello
@drakchaurasia
@Canal1point5
Summary seems to be that Paxlovid simply pauses the viral replication process - once it wears off - in 2-8 days the process continues - remnants in cells are used to synthesize whole live virus again
which has been reported to infect others again (!)
1
4
19
22
13
77
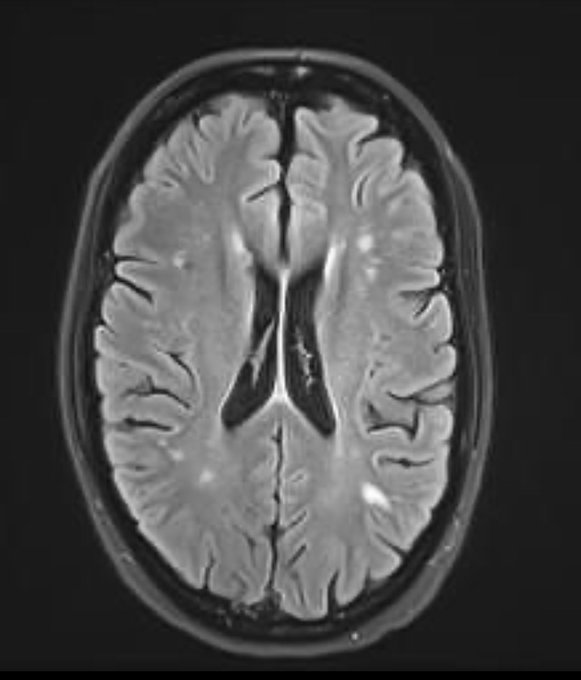
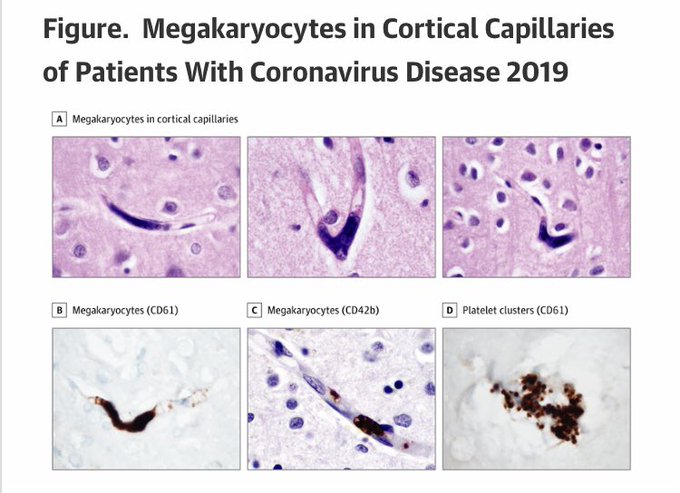
Example of “COVID brain”.
I advise trying to avoid getting COVID for as long as possible, at least until we know more about methods of preventing and treating lasting effects of the disease. Research is in progress, but we still don’t know enough about this.
14
34
78
@loofymectin
@LongTiredRoad
@BernieDogs4
@farid__jalali
@AlisaValdesRod1
I think it is very likely that many people with long COVID have hyper-activated platelets which periodically release large amounts of serotonin. SSRIs can prevent platelets from loading up on serotonin, but that will take time since some platelets would be fully loaded already…
9
15
79
@ShaneyWright
Maybe I can talk to some of my WashU ophthalmology colleagues and see if they are interested in looking into this.
2
1
76
@frothtimus
@farid__jalali
EUA application for use of fluvoxamine to treat early COVID was submitted to the FDA, but it could take months for FDA to review that. Omicron is here now, so it makes sense for doctors to just go ahead and prescribe it off-label now, at least for certain high-risk patients.
5
15
74
@Canal1point5
@SerpinaLonghaul
@YochaiReemMD
@MrsProctor2010
@PeterHotez
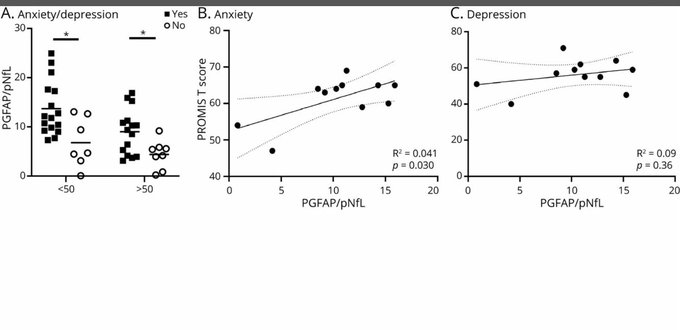
In this study, long COVID patients with higher “anxiety” tended to also have higher evidence of neuronal damage. So, high anxiety should be a reason to assess and address the neurological dysfunction that could be causing the anxiety.
4
22
72
@MVGutierrezMD
@PutrinoLab
This is true. I had COVID 3 times, Acute COVID symptoms were not as bad 2nd and 3rd time, but long COVID gets worse after each re-infection and then gradually improves to near-baseline over 5-6 months each time. I have heard similar stories from other people.
5
14
73
@LongTiredRoad
@AlisaValdesRod1
Also, many people with severe acute COVID have antibodies to serotonin 5-HT2A receptors, and these antibodies may activate those receptors as if they were serotonin. In this case a drug blocking that receptor (perhaps cyproheptadine or mirtazapine) might help.
5
15
68
@fasc1nate
@Ultracaustique
Here's what spicebush swallowtail caterpillars do if you tap them on the back. They stick put this weird Y-shaped smelly appendage that looks like a snake's tongue.
5
3
64
We need more COVID treatment options like fluvoxamine, especially considering the treatment-resistant COVID variants that have emerged. I'm glad to see that Platforma Catracha has been proactive in providing evidence-informed early COVID treatment for the people of Honduras.
9
14
70
@dr_leshan
@farid__jalali
Will be nice to see the full results. I do think timing of treatment may be very important with fluvoxamine. Easier to stop inflammation before it gets far enough along to do significant damage.
4
11
67
PCPs: It really is a good idea to treat outpatients with COVID very early! You might even be able to help prevent overloading of ERs and hospitals!
8
10
69
I'm discussing “Mechanisms of Repurposed Drugs for COVID19” with
@PierreKory
,
@DrRomie
, and 2nd Time Around. Saturday, Jun 12 at 9:00 AM CDT on
@clubhouse
. Join us!
18
18
64
Long-haulers who have had Novavax:
What is your experience with Novavax vs other COVID shots? Do NOT answer unless you have (or have had) Long COVID and have had Novavax.
SE=acute vaccine side effects (1st 2-3 days after shot), LC=long COVID symptom status since shot.
less SE, LC improved
31
less SE, LC stable
29
less SE, LC worse
3
same/worse SE, LC worse
9
14
27
66
Well, I worked hard, along with
@EricLenze2
and many others on our STOP COVID 1&2 teams, but it was Ed Mills & his
@TogetherTrial
who ultimately got fluvoxamine over the line.
7
8
63
It looks like I never actually retweeted this, even though
@__ice9
requested all followers to do so, and I think this is potentially very important. Better late than never.
1
14
64
I’m thinking we really need to accelerate trials of existing drugs repurposed to treat COVID. Vaccines may not be enough to get this under control any time soon.
9
16
65
@Canal1point5
@SerpinaLonghaul
@YochaiReemMD
@MrsProctor2010
@PeterHotez
In other words, anxiety should perhaps give stronger reason for proper assessment and treatment of potential CNS damage, rather than a reason to discount a long COVID patient’s symptoms as being caused by anxiety.
4
8
63
@nihillmatic
Did not take fluvoxamine for the first infection in March 2020. I thought of the idea while sick, but it was just a hypothesis at the time. I did take fluvoxamine the other 2 times. Also been taking it for long COVID, and I increased to max dose for acute COVID. Seems to help.
10
5
62
@richardemoe
@eongmobl
@loofymectin
@drbeen_medical
@EduEngineer
@Same_Sarikei
@Covid19Critical
@chrismartenson
@DrTessaT
@fynn_fan
@DCGreenZone1
@farid__jalali
@deNutrients
I believe in evidence-based medicine, but some EBM proponents look at mortality results like this and interpret this as evidence for NO effect because p-value is not less than 0.05, even though the point estimate suggests there most likely is an effect, but study has low power.
6
11
61
@star9girl9
@YoDoctorYo
Might help to tell your PCP fluvoxamine is in the Johns Hopkins treatment guidelines.
3
15
60