Ruey Hu, MD, MPH
@ruey_hu
Followers
1,840
Following
2,458
Media
232
Statuses
1,890
#ComputationalCardiology , PGY-6 @YaleCardiology from 🇨🇦, @Princeton , @JHUWelchCenter , @VUMCMedicineRes , @KidneyInCVD Supporter
New Haven
Joined July 2013
Don't wanna be here?
Send us removal request.
Explore trending content on Musk Viewer
WE ARE!
• 978449 Tweets
#BUS_แค่น้องชาย_MV
• 220774 Tweets
ORM TIKTOK FASHION SHOW
• 94067 Tweets
クロリンデ
• 69552 Tweets
東京ダービー
• 60546 Tweets
#ENGLOTxATIPAxTIKTOKSHOP
• 46838 Tweets
ファンタジースプリングス
• 34744 Tweets
バレーボール
• 33931 Tweets
配信イベント
• 23489 Tweets
ラムジェット
• 19446 Tweets
ディズニーシー
• 18606 Tweets
アルハイゼン
• 16489 Tweets
THE FANTASY BEGINS
• 16017 Tweets
#神域リーグ2024
• 13743 Tweets
DAOUOFFROAD ON RUNWAY
• 12330 Tweets
アンモシエラ
• 10615 Tweets
危機契約
• 10599 Tweets
Last Seen Profiles
Congrats
@nathanwchen
on a great senior thesis on novel somatic variants in human disease! And congrats to all
@yaledatascience
seniors on a very, very diverse set of projects. 👏👏👏
@jennkwanMDPhD
Congrats
@nathanwchen
on presenting 1) your senior thesis work evaluating CHIP/novel somatic variants & their effects on human disease! 2) Using Q learning on simulating optimal figure skating ⛸programs to maximize scores
@Yale
@yaledatascience
What a milestone!
3
144
341
1
108
235
I am thrilled and overjoyed to have matched into cardiology fellowship at
@YaleCardiology
!
I am grateful to Dr
@edwardmillermd
for welcoming me to my next home and
@DrJohnMcP
for 3 incredible years learning and growing at
@VUMCMedicineRes
26
3
184
Thrilled and honored to learn that I've been named one of the 28
#StatWunderkinds
for 2023!
My gratitude 🌟 goes to ALL of the medical students, residents, fellows, and faculty at
@YaleCardiology
@YaleIM_Chiefs
@YaleIMed
@VUMCMedicineRes
@JHUWelchCenter
and elsewhere who has
17
9
149
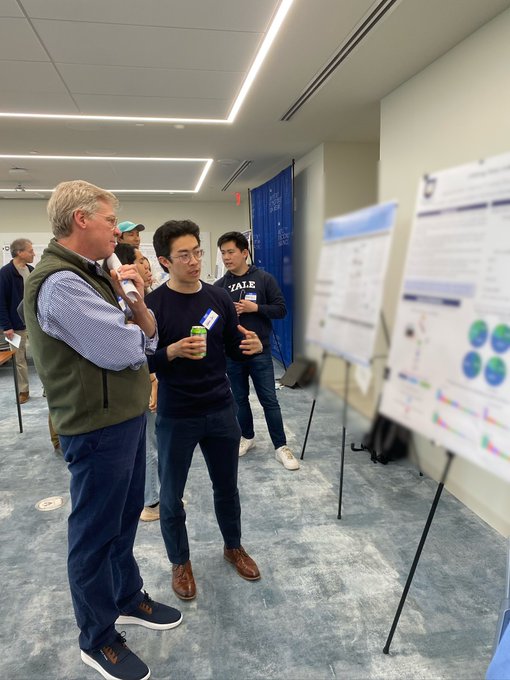
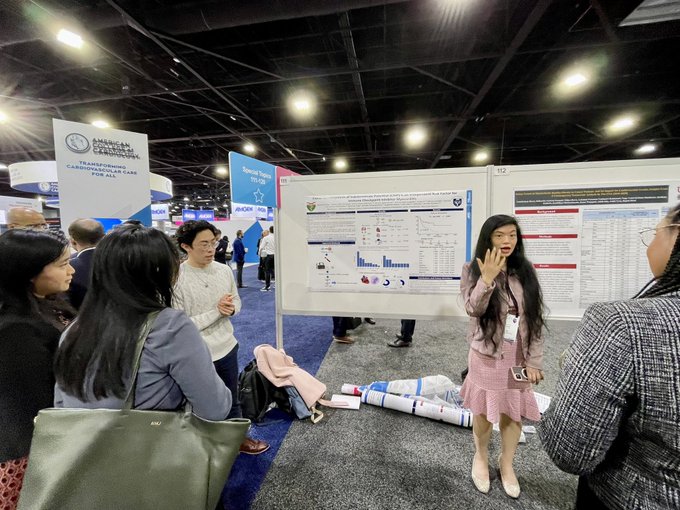
Engaging crowd as
@nathanwchen
and
@jennkwanMDPhD
show their data that clonal hematopoiesis of indeterminate potential is a risk factor for ICI myocarditis at
#ACC24
@nonajiang
@DrToTheRescue
@MandanaChitsaz
@Sarajdiaz1
1
63
149
Thank you for this honor and surprise
@yaleem2
! I hope/promise to be kind to every one who consults! 🫀💖💓
@YaleCardiology
Jiun-Ruey Hu, MD, MPH, was voted as Consultant of the Year by residents and interns of the
@Yale_EM
at the Yale School of Medicine.
Read more about his career as a clinician-educator:
1
5
47
11
9
110
Belated, but so happy to get my copy of
@HTNSecrets
in the mail at last! 🎁 Thank you
@DrJMLuther
@hswapnil
@edgarvlermamd
for letting me contribute! Alongside some of my favorite people in the kidney🫘 bean world
4
2
72
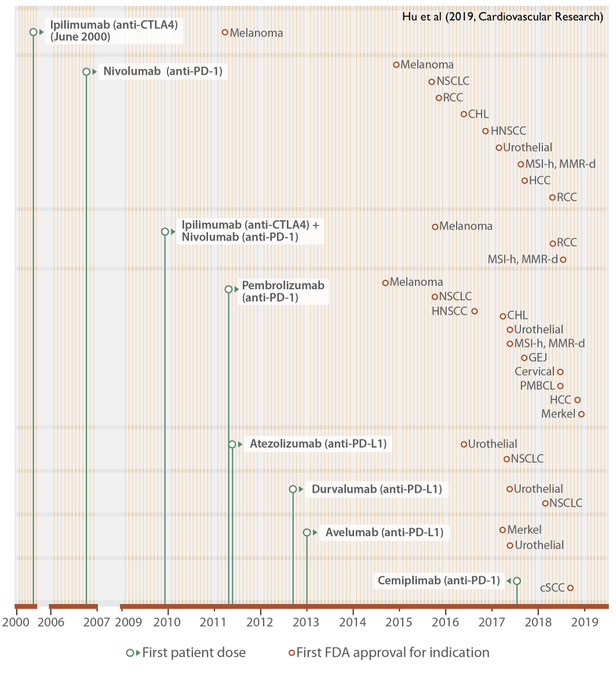
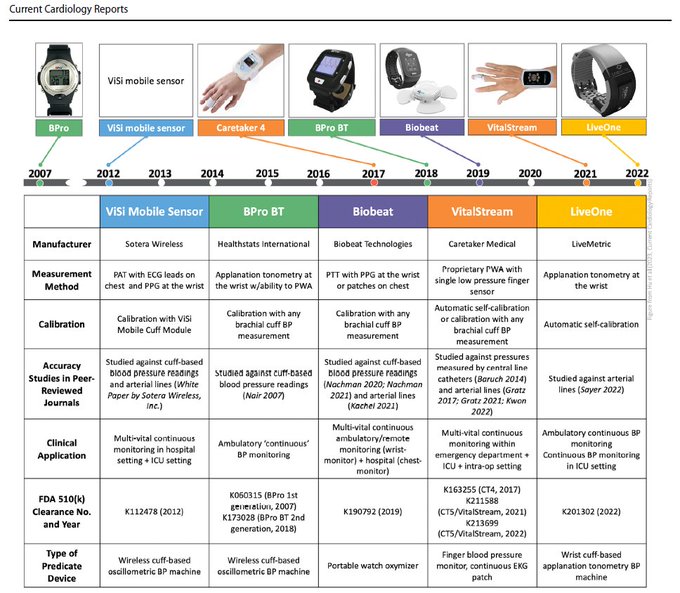
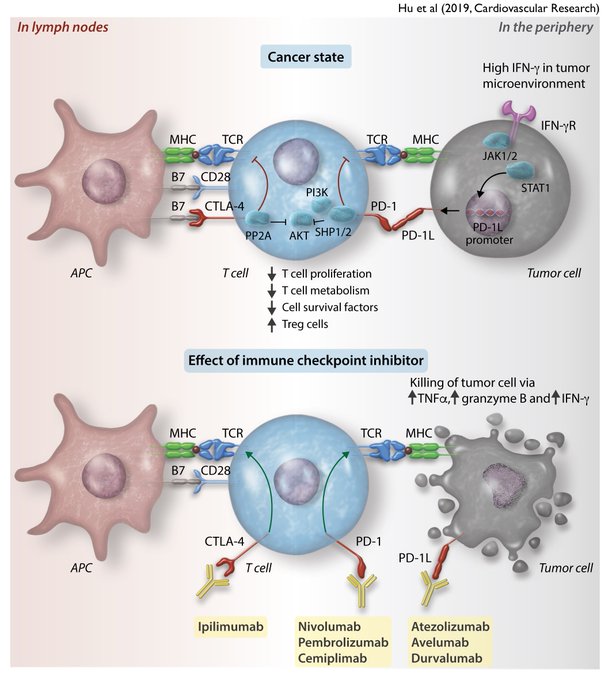
Here's a quick reference of immune checkpoint inhibitors available today and their latest
@FDAOncology
-approved indications.
Yellow line = month, green dot = drug, brown dot = use.
#DataViz
from
@VUMCHemOnc
@HopkinsKimmel
@VUMC_heart
@hopkinsheart
@CardioOncology
2
46
69
Weekend teaching about why bundle branch blocks look the way they do by
@Milesshen8
in the CCU
#AlreadyAFellow
@YaleIM_Chiefs
@ElliottMillerMD
0
0
62
So happy to be teaching the residents & students who have rotated through. Can't wait to work with more of
@YaleMed
&
@YaleIMed
in the coming months!
Sanchez, Rege, and Hu Honored with Teaching Awards via
@yalemed
Congratulations to 1st Year Fellow,
@ruey_hu
, for this recognition of his fantastic teaching skills!
@YaleCardiology
1
2
37
9
1
59
Rising interns
#Match2024
and sub-interns in internal medicine
#Match2025
, interested in practical tips to approach common issues in internal medicine? Come listen to
@TradIMYale
residents Drs
@SanjuGarimella
@RamyaSampathMD
@ArshKhokhar_med
and Stephanie Kim
@YaleIMed
Incredible,
@ruey_hu
and thanks for asking our
@TradIMYale
residents to participate!
@YaleIMed
@SanjuGarimella
@RamyaSampathMD
@ArshKhokhar_med
and Stephanie Kim!
0
2
12
0
16
59
Thanks to the wonderful team & friends☺️ of the
#Troponin
Toolbox at
#ACC24
Special shout out to
@daeyongp92
and
@ZacharyYeMed
for analyzing the data and presenting.
@YaleCardiology
@YaleIMed
@TempleIM
4
8
57
You've heard of Choosing Wisely. Now, we present to you: Stressing Wisely!🏃♀️
Congratulations 🎉🥂 and thank you to Drs
@camilatrejop
, Wright, Esin,
@attilafehermd
@edwardmillermd
and soon-to-be Dr Maayah
@YaleMed
for bringing this idea to life. Thank you to ASNC for the National
The American Society of Nuclear Cardiology (
@MyASNC
) named a
@YaleCardiology
team winners of the 2023 National Quality Improvement Challenge for their digital clinical decision support tool.
More on the tool Stressing Wisely ⬇️
@edwardmillermd
@ruey_hu
0
2
11
4
6
52
I'm so grateful to
@CarlosMenaYale
and
@KimGSmolderen
who are visionary and thoughtful mentors! More to come!
Congrats to
@ruey_hu
for his travel award during
@AHAMeetings
@CouncilPvd
We are blessed with incredibly talented FIT
#PAD
@YaleCardiology
@KimGSmolderen
@edwardmillermd
@Yale
@YNHH
1
3
26
5
5
50
.
@David_Ouyang
is someone I have looked up to for many years. So grateful to work together on machine learning in cardiology.
2
0
47
Thank you residents
The Department of Internal Medicine’s 2022 Fellow of the Year is Ruey Hu, MD, MPH. At Yale,
@ruey_hu
has helped mentor medical students and residents on research and medical education projects.
Learn more:
@YaleMed
@YaleIMed
@edwardmillermd
1
3
37
2
0
44
Our med student Dan Grubman giving us a chalk talk on coronary angiography projections with a cup. I will never be able to draw like this!
#Impressed
@ASanchez_PS
@ElliottMillerMD
@Cory_naryCareRx
1
3
43
Thank you
@isabellacueto
for publishing this nice interview in
@statnews
today! It was such a pleasure to meet all of your colleagues including
@SciFleur
@GideonGil
@sarahmupo
@fitzcodder
@elaineywchen
@cmilz3211
and others (:
Cardiologist Ruey Hu (
@ruey_hu
) is a Renaissance man. He plays 4 instruments, was in an East Asian acapella group in undergrad. He composes music, ice skates, does tae kwon do.
And he's hand-coding innovative tools for doctors.
#STATWunderkinds
0
4
22
3
6
41
It is my greatest pleasure to mentor everyone with an interest in
#ComputationalCardiology
! Thank you Dr
@MarkDSiegel1
for creating such a collaborative environment for
@TradIMYale
residents, who have really stepped up to the challenge!
Indeed! The future of digital decision support, right here in
@YaleIMed
and
@YaleCardiology
Thank you
@ruey_hu
for including so many
@TradIMYale
residents in your work!
0
3
31
0
1
38
Nice to get to see Dr
@ErinMichos
as part of the Dr Lynda Rosenfeld Visiting Professorship
@YaleCardiology
! Thank you for the advice to the fellows
@ekoikonomou
@rraven8
@AmarMD99
@LScierkaMD
@NNShahMD
@George__GH
1
4
37
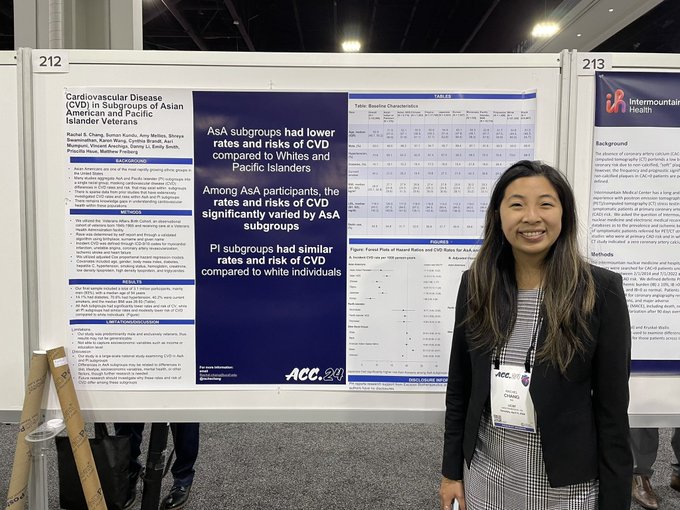
Rates and risks of CVD differ significantly by Asian American and Pacific Islander subgroups. Another reminder of the importance of disaggregation. Check out this
#ACC24
poster by
@rachechang
from
@UCSFIMChiefs
0
2
36
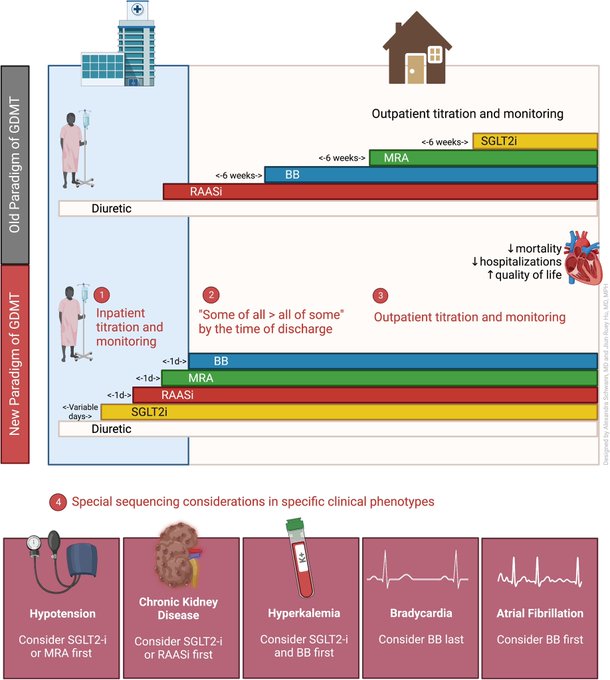
The role of quadruple
#GDMT
💊 in patients with🫀 heart failure with reduced ejection fraction is widely accepted. But does the *sequence* and *speed* with which we initiate GDMT matter? 🤔
📝 is there a “PEMDAS” for GDMT sequencing in HFrEF? 🤔💊🫀
🆕 practical review led by
@ruey_hu
,
@aschwann212
,
@jiiiiawei
,
@abdulelahnuqali
, &
@MHBeasleyMD
🔗 open access ➡️
1
17
38
2
6
36
Blood pressure fluctuations *outside* the clinic setting are associated with risk of stroke (Kario, 2023, Hypertens Res), but current intermittent cuff-based BP devices, including home and ambulatory devices, are unable to capture the breadth of BP
variability across activities.
Delighted to share our new review on cuffless devices led by
@YaleCardiology
fellow
@ruey_hu
posted online today:
2
21
65
1
9
36
Come to poster 34 at
#ACC23
@ACCinTouch
to learn about
#GDMTforEveryone
!
@jiiiiawei
@YaleCardiology
1
3
35
Thank you for welcoming us to our new home
@YaleCardiology
Welcome new first year Yale Cardiovascular Medicine Fellows!
@YaleCardiology
@andishahu
@ingahlif
@ekoikonomou
@ruey_hu
@MaxwellDawson13
2
6
72
1
1
34
Hey
#CardioTwitter
! Check out this
#HFpEF
trial by Dr Kavita Sharma and colleagues
@HopkinsMedicine
hot off the press in
@JACCJournals
– Randomized Evaluation of
#HFpEF
Patients With Acute Heart Failure and Dopamine
1
13
32
I wanna give a shout out to the 🌠 resident who carefully combed through hundreds of papers for this effort with me, Jiawei Tan.
#NephTwitter
#ERAS2023
fellowship PDs, please consider her! 🙏
If you have patients with CHF, please check out created by our stellar fellow
@ruey_hu
. Simply amazing interactive educational website.
@YaleCardiology
@YaleHF
@ericjvelazquez
@yaleHFdoc
6
18
97
2
1
31
Nice job by soon-to-be cardiology fellows
@evivemmou
@INikolakopoulos
Omar El-Charif and Justin Dwyer
@YaleIMed
at Yale GME talent show!
1
7
31
Very happy to be speaking about the collection of
#ComputationalCardiology
tools that we have designed to improve uptake of guidelines and evidence-based medicine in cardiology, at the Emirates
@CardiacSociety
/Asian Pacific Society of Cardiology
@apsc_office
@YaleCardiology
1
3
31
Thank you to all the exceptional student leaders including
@donnatranmd
and
@msJoyceLee
who put in tireless work to advance the mission of
@APAMSA
. Thank you to all the residents, fellows, and med students
@YaleIMed
@YaleMed
who have directly contributed to the effort.
A lovely tribute to a spectacular
@YaleCardiology
fellow! Congratulations,
@ruey_hu
!
Hu Receives National Mentorship Award via
@Yale
Cardiovascular Medicine
@DrJohnMcP
@YaleIMed
7
6
75
3
2
31
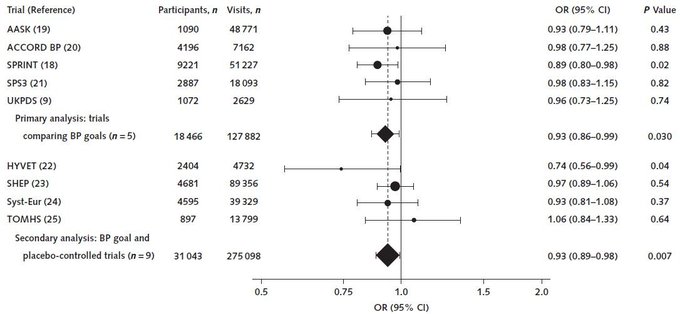
Concern about risk for orthostatic hypotension should not in itself be a reason to avoid or de-escalate treatment for
#HTN
Check out this meta-analysis of AASK, ACCORD BP, SPRINT, SPS3, UKPDS, HYVET, SHEP, Syst-Eur, and TOMHS led by Dr
@spjuraschek
@BIDMC_GenMedRes
@AnnalsofIM
New systematic review published in Annals of Internal Medicine suggests that
#hypertension
treatment lowers the risk for orthostatic hypotension, or extreme drop in
#bloodpressure
upon standing.
Read more .
0
10
28
6
7
31
Beautiful feature on my mentor Dr
@meg21212
’s prolific young career as she receives the
@ASNKidney
@AHAMeetings
Donald W. Seldin Young Investigator Award at the closing plenary of
#KidneyWk
2
8
30
@Nephro_Sparks
@KidneyInCVD
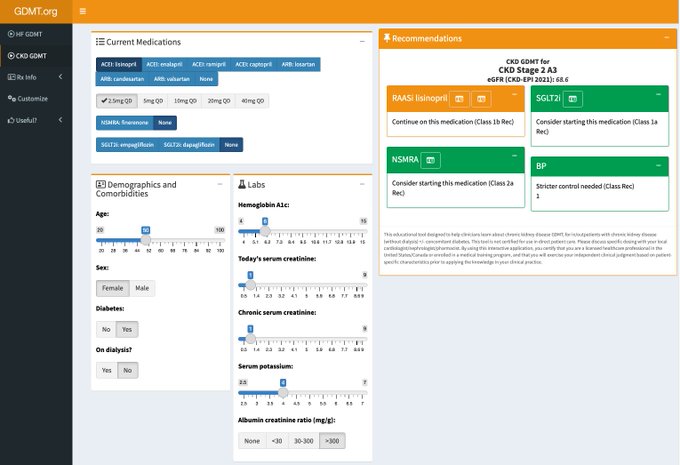
In the 2024 update to , we integrate the
@goKDIGO
guidelines to help increase the uptake of evidence-based therapies for slowing CKD progression.
Thank you Drs
@Nephro_Sparks
@LeslieGewin
&
@RangaswJ
for the opportunity to speak
@AHAScience
@KidneyInCVD
3
15
28
CONGRATULATIONS to my friend and talented fellow Dr Devika Nair
@devimol
for placing 2nd at the National Young Investigators' Forum in Clinical Science
@NKFCLINICALS
!
@VUMCKidney
Spirit! 🏅🎉
7
6
28
Only 1 in 8 patients with cardiovascular disease are diagnosed before the onset of symptoms, Dr
@rohan_khera
notes
@CVCTForum
.
Work from
@cards_lab
@YaleCardiology
by
@LovedeepDhingra
@ekoikonomou
@PhyllisTweets
@Veer_Sangha_
@AryaAminorroaya
@aakhunte
has shown that
#AIECG
can
1
8
26
CuffLESS blood pressure measurement devices offer the promise of outpatient beat-to-beat🫀monitoring, but regulation has failed to match the pace of innovation
@CVDH_journal
:
@spjuraschek
@lckovell
@TammyBradyMD
@rantocran
@YaleCardiology
@DigiCard10MD
Our commentary on validation protocols for cuffless BP monitors is in press, led by the brilliant
@ruey_hu
with
@lckovell
@rantocran
@TammyBradyMD
...
Read our thoughts on what validation should look like!
Validating cuffless blood pressure devices
2
10
21
1
6
28
Thank you
@jiiiiawei
for running with me on this idea when it was a seedling! 🌱🌻
8
2
26
I could not have dreamed of a better partner than my friend Rochelle Wong MS3
@VUSM
for this yearlong quality improvement project. Today we won the
@ACPinternists
National Medical Student Abstract Poster Competition among 150 finalists at
#im2018
! PDs, please consider Rochelle :)
1
2
26
.
@ekoikonomou
presenting at
@ACCinTouch
:
@cards_lab
ASSIST tool recommendation for CCTA was associated more severe anatomical disease and intensification of preventive therapies, which may explain the prognostic value of ASSIST
0
4
27
Can't get enough of metabolomics! 😅 Thank you
@DrTariqShafi
for mentoring me on this exciting research, Drs
@JoeCoresh
&
@meg21212
for mentoring me on prior metabolomics projects, Dr Myint for her ML acumen, and all coauthors Drs
@LAInker
@ASLtufts
Guallar, Hansen & Rhee
Congratulations to PGY3
@ruey_hu
who placed 1st at the Mid-Atlantic Young Investigators' Forum for his research on uremic symptoms and the serum metabolome! Ruey will represent
@VUMCKidney
@VUMCMedicineRes
at the national competition
@NKF
in April.
2
2
36
2
1
25
Do metabolites associate with mortality in chronic kidney disease (beyond usual suspects)? Check out our new study in MDRD & AASK!
Thanks mentors
@meg21212
@JoeCoresh
@ASLtufts
@LAInker
@LarryAppel
@JHUWelchCenter
@hopkinsneph
@TMCNephFellows
@Kidney_Int
5
10
26
Every minute I listen to Dr
@ErinMichos
she osmoses another pearl of career wisdom. Can’t wait for her keynote today
@AHAMeetings
#EPILifestyle19
#mentorship
#sponsorship
Hello to more
@CardioOncology
collaborations
1
4
26
Had a great time speaking with
@KHRC_research
@UCSFNephrology
about ideas for
#ComputationalNephrology
💡.
Thank you Dr
@jlampre
for the invitation! Thank you Dr
@estrella_khrc
@shlipak_khrc
@JamshidianMitra
for the insightful discussion.
2
3
26
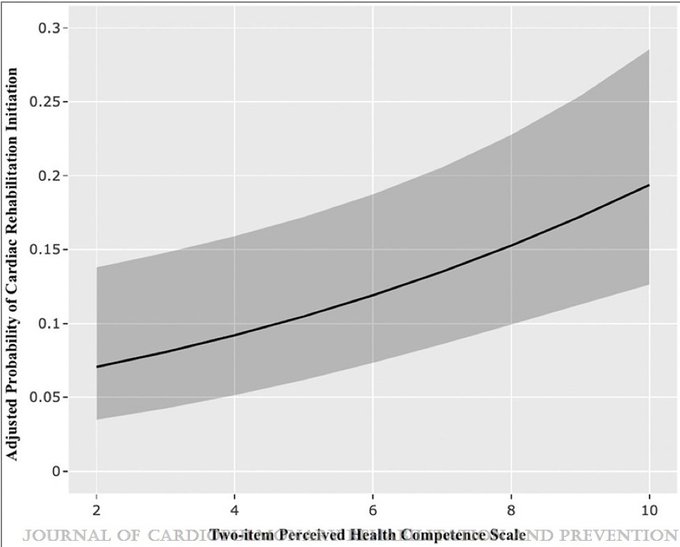
<25% of eligible patients initiate🫀cardiac rehab after MI or HF 🏥.
PERCEIVED health competence–belief in one's ability to achieve health-related goals–is a psychological factor🧠strongly associated with likelihood of initiating cardiac rehab.
@JCRPjrnl
2
1
25
Dr
@SpatzErica
@YaleCardiology
outlines the change we need to see in the future of blood pressure monitoring
@AHAScience
@HyperAHA
:
1️⃣ Validation of novel cuffless BP devices in diverse populations
2️⃣ Utilization of contextual data to identify contributing factors for
0
2
24
In
@JAMANetworkOpen
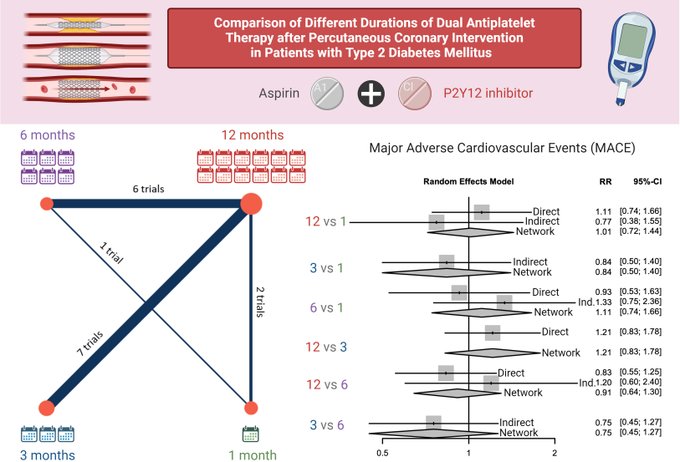
today: Older adults (>65/>75yo) are simultaneously at the highest risk for MACE and also bleeding.🩸What is the optimal duration of DAPT in older adults after PCI?
Please check out this
#SystematicReview
and Network
#MetaAnalysis
of 14 RCTs by
@daeyongp92
1
5
23
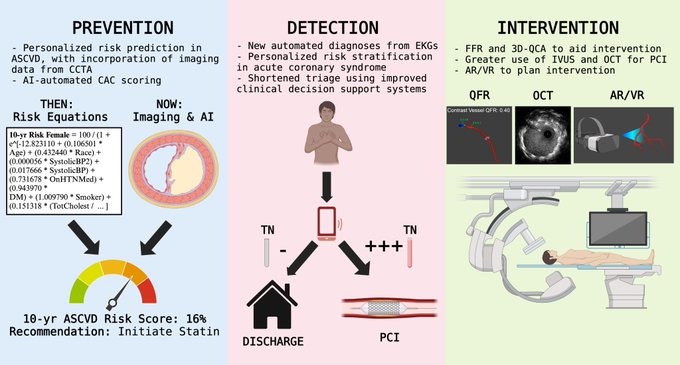
What digital tools can assist in decision-making in acute coronary syndrome?🧵
Validated scores readily available on
@mdcalc
include:
GRACE:
HEART:
HE-MACS:
T-MACS:
The GRACE ACS
Smartphone- and web-based digital aids can bring evidence-based risk estimation models to the point of care. Proud of
@YaleMed
students
@see_laudia
,
@ScottGrubman
, and Daniel Grubman for putting together this review on digital tools for decision-making in coronary artery disease,
0
4
16
1
2
25
Congratulations Dr
@samitshahmd
for receiving the Dr Lynda Rosenfeld Award for mentoring and teaching fellows! Nominated by
@mytachybrady
@SteffneK
0
2
23
The highlight of my
#ACC23
is catching up with
@Sugeng_Lissa
, who has mentored generations of Yale fellows, even from afar
2
0
23
"Keep running. If you've never gotten a paper rejected, you've never submitted one." -
@AASLDtweets
president Dr Anna Lok
0
8
22
Congratulations to Drs
@DrDeidraCrews
,
@stephensozio
and all others on well-earned ASN Mid-Career Awards!
#KidneyWk
PC: Dr
@oakparkben
1
3
23
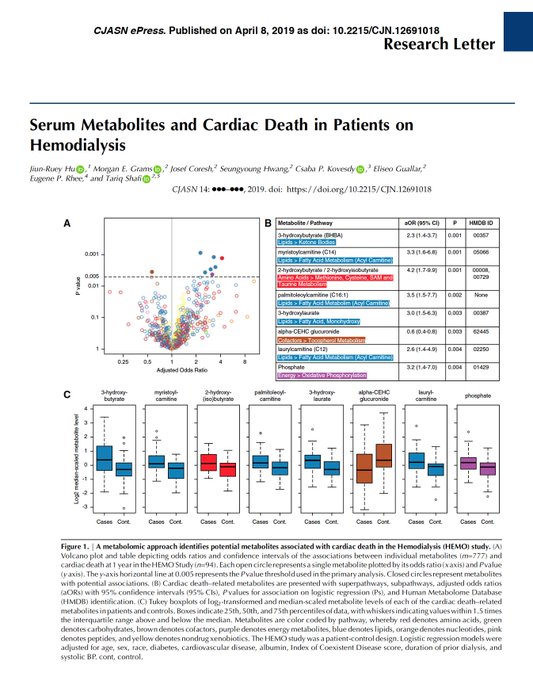
Ever wondered about metabolites and cardiac death in ESRD? Here's what
@DrTariqShafi
and I found in the HEMO study!
– with thanks to Drs
@meg21212
@JoeCoresh
Csaba Kovesdy
@EliseoGuallar
& Eugene Rhee
@CJASN
2
3
22
Can
#ComputationalCardiology
tools be useful in global health settings? Tune in this Friday March 15th, 2024. Thank you to the El Salvador National Institute of Health
@INS_ESV
&
@YaleCardiology
Drs McNamara, Lombo, and
@rraven8
for the invitation.
El INS y
@YaleCardiology
de la
@Yale
invitan a participar en modalidad virtual, en el Simposio Cardiovascular, a realizarse el viernes 15 de marzo, 2024, a partir de las 9:00 a.m. desde el INS.
0
1
3
1
4
20
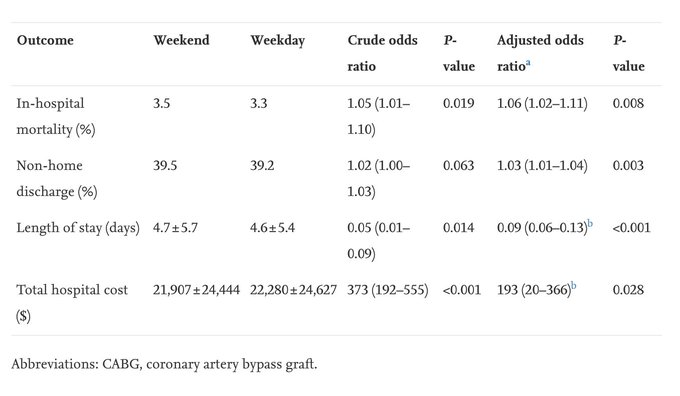
Unfortunately, weekend NSTEMI continues to have higher in-hospital mortality, decreased PCI rates, and longer LOS than weekday NSTEMI.
@CRMjournal
with
@daeyongp92
@MichaelGNanna
@YaleCardiology
@VijAviral
@ChanavuthK
@KhawarSana
Contemporary weekend effect on management and in-hospital outcomes of
#NSTEMI
by Dae YongPark at al.
1
5
11
0
4
22
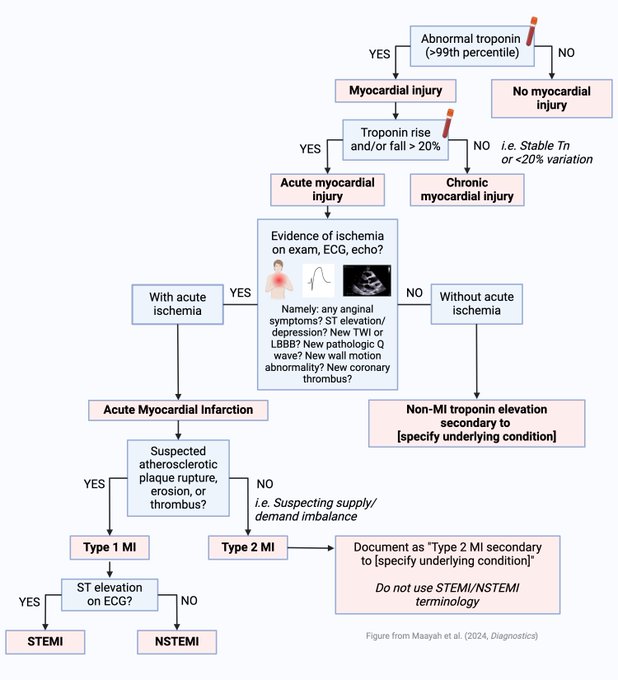
Check out this paper by Maayah
@ScottGrubman
Allen
@ZacharyYeMed
@daeyongp92
@evivemmou
Gokhan
@WSunMD
Possick
@jennkwanMDPhD
Gandhi
@ruey_hu
from
@YaleCardiology
@YaleIMed
@yaleem2
where these illustrations are from.
1
3
20
Great advice from
@ErinMichos
@AnumSaeedMD
@amehta_09
about the transition from fellow to early career faculty at
#AHA23
moderated by
@PrernaGuptaMD
@s7saith
1
2
19
Jeopardy/Cupcakes (🤩!!) by Dr Freed to wrap up an incredible week of learning on the resident cardiology service
@YaleIMed
🫀
@YaleCardiology
0
2
21
If you are entering residency in any of these specialties or preparing for a sub-I, please register below to watch! We are working hard
@APAMSA
to put together quality review content for you!
1
1
20
Breaker of both glass and bamboo ceilings
@umichmedicine
Dr Anna Lok
@AASLDPresident
@AASLDtweets
receives the 2017
#CAMS
Scientific Award
1
5
21
Another full house for artificial intelligence trials
@CVCTForum
, cochaired by Drs
@rohan_khera
&
@girish_nadkarni
. Upcoming talks by
@PhyllisTweets
@hmkyale
@jbmortazavi
@YaleCardiology
2
5
20
#GDMT
reduces mortality and hospitalizations but is consistently underutilized, especially in patients with concomitant
@KidneyInCVD
. Back in 2022,
@jiiiiawei
@StanfordNeph
and I created an educational tool to assist in decision-making for GDMT in
#HFrEF
.
1
5
19
@djc795
@kellycardiology
@nyphospital
@ColumbiaMed
Yes! And all the community hospitals that struggled with getting resources but never make it to the news or thank you list
1
0
19
An honor to meet the one and only Dr
@KBibbinsDomingo
@JAMA_current
. Thank you for your time and advice.
0
0
20
@ekoikonomou
and colleagues at
@cards_lab
@YaleCardiology
have developed an automated end-to-end machine learning phenomapping-guided algorithm for adaptive,
#PredictiveEnrichment
of RCTs.
The algorithm can be defined at the protocol stage without any a priori knowledge and no
0
6
19
Half the credit belongs to
@jiiiiawei
@StanfordNeph
for GDMT for Everyone. Thank you
@RamyaSampathMD
for coming to Grand Rounds, and congratulations on your paper on goal-concordant ESKD decisions!
@KidneyInCVD
Absolutely stunning Grand Rounds from
@ruey_hu
😍 Pretty sure I’ll be using this tool everyday.
2
2
12
0
4
20
Medical students, ever wonder what to make of 🫀 telemetry?
Join National
@APAMSA
this Saturday, May 18th from 2-4 PM PT (5-7 PM ET) for our EKG & telemetry workshop by Frank Qian
@frankq1368
@BUCards
& Alex Choy
@MSHCardsCT
(incoming EP fellow)
✏️Register now at
0
5
20
Take home points from
@Carlos_DavilaMD
@YaleCardiology
about mechanical circulatory support devices in cardiorenal syndrome
@AHAScience
@KidneyInCVD
:
1️⃣ Acute MCS devices are increasingly used in CRS
2️⃣ Defining and reporting renal outcomes in patients receiving acute MCS remains
0
4
20
Dr
@CarlosMenaYale
opens the
@Yalecards
Interventional Cardiology Symposium discussing controversies in drug-coated technologies
@NHLawnClub
with
@YousifAhmad
as co-course director. Exciting lineup!
0
0
19
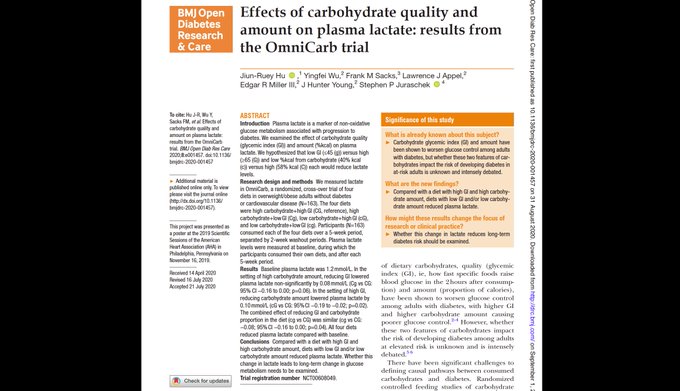
Carbohydrate glycemic index & amount worsen glucose control among adults with diabetes, but whether these 2 features of carbohydrates impact the risk of *developing* diabetes is debated
@BMJ_Open
@BIDMC_GenMedRes
@JHUWelchCenter
@VUMCMedicineRes
@NYUIMRes
3
4
19
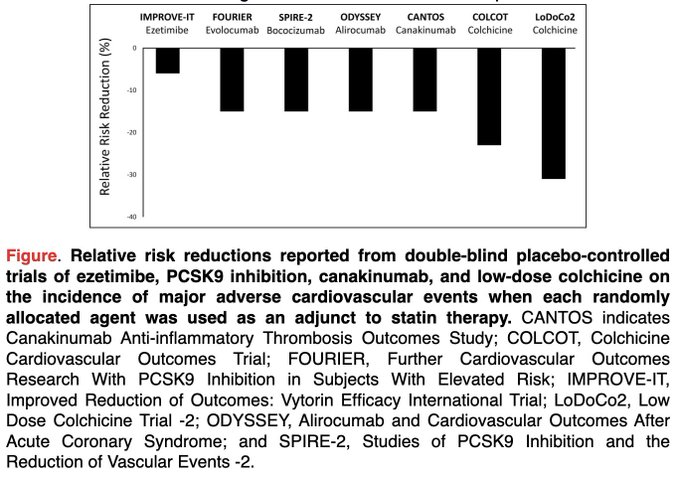
Dr Paul Ridker at Brigham
@bwhcvls
points out
@CVCTForum
that the relative risk reduction in MACE in double-blind placebo-controlled trials of colchicine excdeeded that of PCSK9 inhibitors and ezetimibe as an adjunct to statin therapy.
2
2
18
Shout out to Drs
@camilatrejop
@DrKene
@DrMCTan
@ScottGrubman
@jfreeMD
and others not on twitter for their work on developing the Afib Assist Tool! Thank you for Dr
@AyeshaButtMD
for coming to grand rounds and for your advocacy for IMGs!
0
3
19
Immune checkpoint inhibitors have changed the treatment landscape for
#cancer
patients by inhibiting PD-1, PD-1L, or CTLA-4.
@sitcancer
@ASCO
#ImmunoOnc19
#Immunotherapy
1
9
18
So happy to work (& code!) with talented and motivated individuals like you
@Sarajdiaz1
&
@MandanaChitsaz
! Thank you all for sharing the vision
@ScottGrubman
@carsalpajarillo
Had the pleasure to meet
@ruey_hu
@carsalpajarillo
and Scott from Yale during
#AHA2023
this weekend. Check out Ruey’s incredible app for quick and accessible recommendations on GDMT at !
0
0
19
0
2
18
I am thrilled to have matched at
@VUMChealth
for my Internal Medicine residency. So grateful to my family and my mentors at
@VUSM
@VUMCKidney
and
@JHUWelchCenter
! Three more years!
#Match2018
#MatchDay2018
5
0
18
Just out in
@JAHA_AHA
🗞 , thanks to the 💡mentorship of Drs Chenxi Huang, Murugiah
@murugiah_k
and Krumholz
@hmkyale
@YaleCardiology
and contributions of Drs Lu,
@MitsuakiSawano
, Xin, Messenger,
@Dr_BowTie65
and
@fperrywilson
@YaleNephrology
@KidneyInCVD
1
2
17
Happy birthday Dr
@JoeCoresh
! Happy birthday to the Chronic Kidney Disease Prognosis Consortium! 🎉🍾🎊🎈 Beautiful toasts & hard work planning by Drs
@meg21212
@Shoshana_Ballew
@ASLtufts
Violetta and others
0
1
15
Had a great time presenting this top-scoring late-breaking abstract on
#HPP
at
@TheEndoSociety
#ENDO2018
with
@VanderbiltMSTP
@Juan_Colazo
and our mentors Drs Dahir & Simmons
@VUSM
2
2
17
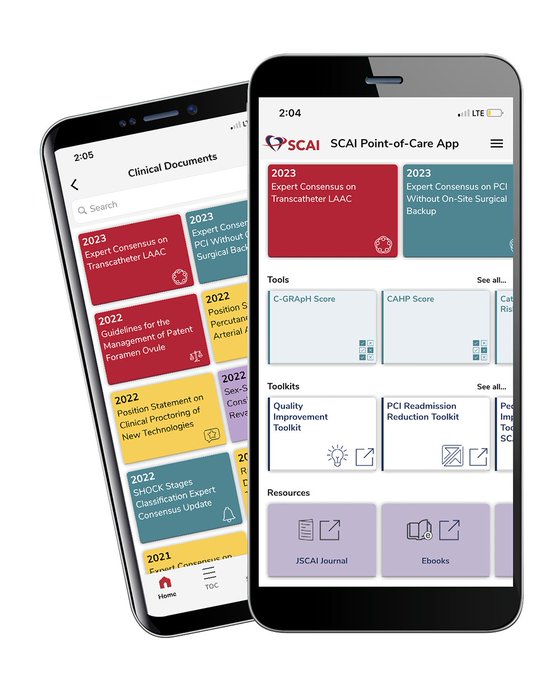
What digital tools can assist in PCI planning?🧵
@SCAI
's Point-of-Care App offers quick access not just to guidelines but also its PCI Risk Assessment Tool, which predicts the risk of in-hospital mortality, bleeding, AKI, and femoral complications. Based on data from Brennan
Smartphone- and web-based digital aids can bring evidence-based risk estimation models to the point of care. Proud of
@YaleMed
students
@see_laudia
,
@ScottGrubman
, and Daniel Grubman for putting together this review on digital tools for decision-making in coronary artery disease,
0
4
16
1
3
16
To read more about the promise and limitations of cuffless BP devices, please check out our review "The Promise and Illusion of Continuous, Cuffless Blood Pressure Monitoring" published today
@SpringerCurRpts
with
@daeyongp92
@spjuraschek
@rantocran
0
4
17
Dr
@hmkyale
opens today’s
@CVCTForum
session on Digital Tools for Trial Design and Execution, cochaired with Dr
@lamcardio
0
4
17
Learn from
@Milesshen8
,
@ArshKhokhar_med
, upcoming CHIEF
@SanjuGarimella
, Akash, and Ysa
@YaleIM_Chiefs
! Register now at
0
4
17
Very interesting to listen to my friend
#STATwunderkind
@brendacabreram
talk about her work on the genetics of psychiatric disorders and populations underrepresented in genetic databases
@statnews
#STATsummit
@YalePsych
0
2
16
Abatacept as an investigational agent for immune checkpoint inhibitor myocarditis? – Check out
@DrJESalem
@mathieukerneis
@CardioOncology
’s case report in
@NEJM
Congratulations to
@DrJESalem
@mathieukerneis
on this terrific
@NEJM
paper! Terrific team now in place
@APHP
for transatlantic efforts 2 better understand immune checkpoint inhibitor-associated myocarditis! Look forward 2 future collaborations!
@VUMC_heart
3
30
79
0
4
16