Bryan Carmody
@jbcarmody
Followers
50,855
Following
942
Media
2,173
Statuses
11,966
The Sheriff of Sodium | Pediatric nephrologist | Associate professor | APD | Husband | Dad | Virginian | Advocate for medical students and common sense
Hampton Roads, VA
Joined July 2013
Don't wanna be here?
Send us removal request.
Explore trending content on Musk Viewer
Kendrick
• 588355 Tweets
Drake
• 522978 Tweets
Rio Grande do Sul
• 258633 Tweets
Madonna
• 184920 Tweets
Ole Miss
• 111110 Tweets
Reus
• 87811 Tweets
Sony
• 76283 Tweets
Star Wars
• 62881 Tweets
PlayStation
• 58235 Tweets
Porto Alegre
• 56771 Tweets
ウズベキスタン
• 41744 Tweets
Hope Hicks
• 28928 Tweets
Starc
• 28865 Tweets
Wankhede
• 21080 Tweets
ブライアン
• 20098 Tweets
الوحدة
• 19952 Tweets
Helldivers 2
• 19106 Tweets
日本優勝
• 16292 Tweets
#الاتحاد_ابها
• 16258 Tweets
Luton
• 15693 Tweets
Lorca
• 14411 Tweets
Henry Cuellar
• 13574 Tweets
Mark Hamill
• 12086 Tweets
Sybil
• 12058 Tweets
#David69
• 10620 Tweets
Keyshia
• 10452 Tweets
Last Seen Profiles
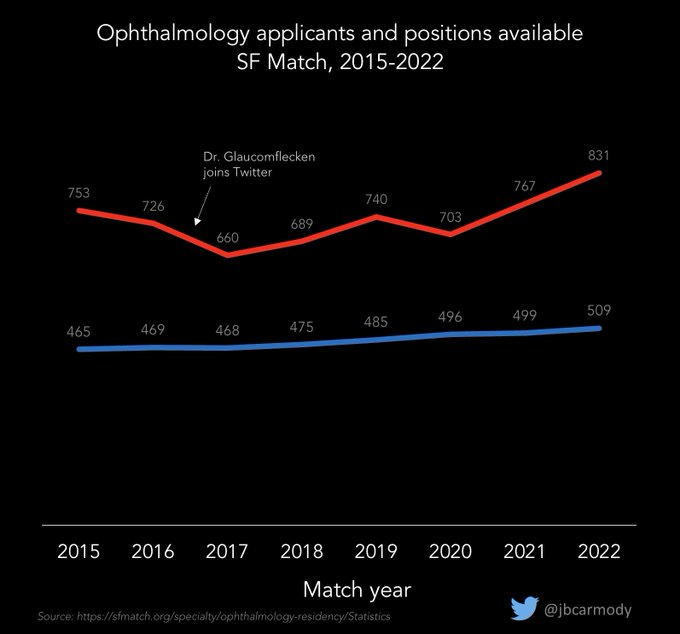
Last year saw a record number of applicants for the opthalmology match.
Let the AAMC talk about the ‘Fauci effect’ in medical school applications - I’m gonna talk about the
@DGlaucomflecken
effect for ophthalmology residency programs.
22
64
2K
It’s one thing for an insurer to DENY a claim. But why do so many insurers expend such effort to DELAY payment, even for justified claims they know they have to pay?
If you didn’t know already, let me teach you about “float.”
(thread)
I’m trying to think of another industry with record profits that just doesn’t pay its bills.
Anthem, UnitedHealthcare, other major insurers are running billions behind in payments to hospitals, doctors via
@USATODAY
26
190
475
45
695
2K
Good Lord.
Suggestions include attending a tuition-free medical school, “improving financial literacy,” and applying to fewer medical schools.
Why not include “Don’t be poor” while you’re at it?
28
280
2K
Hate to be the bearer of bad news, but…
Yes, medical residents are once again exempted from being paid overtime.
See p. 378 of the final rule PDF:
26
264
1K
@DGlaucomflecken
The man is telling the truth.
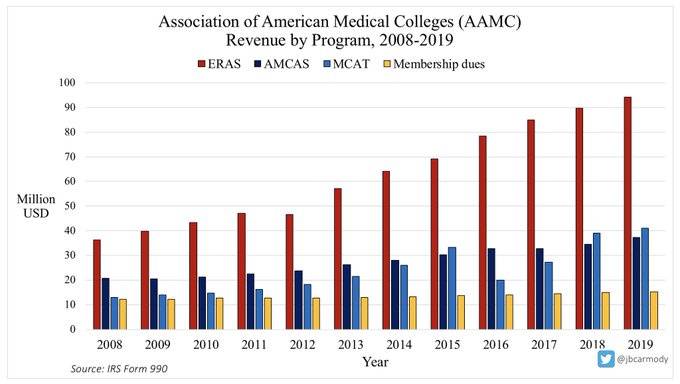
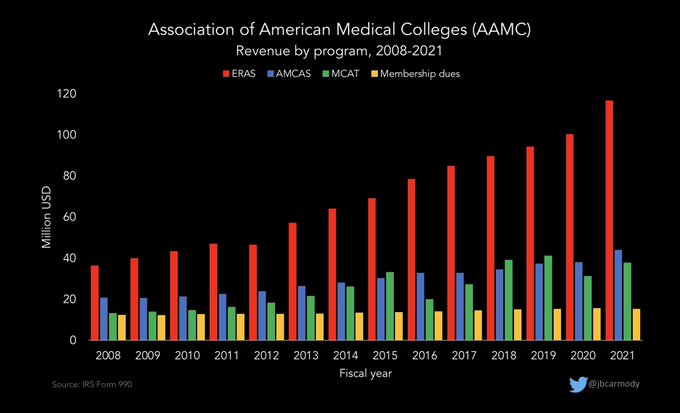
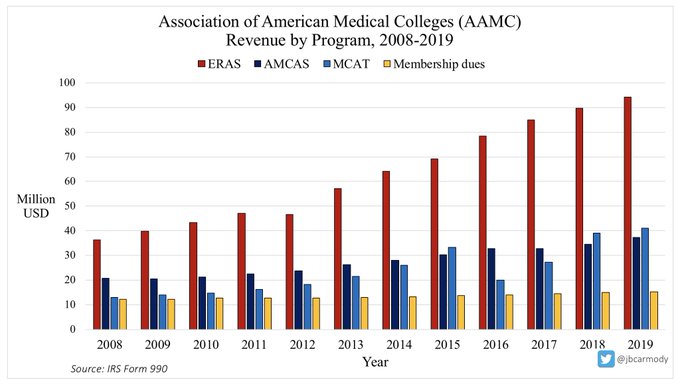
ERAS has become the AAMC’s cash cow, with revenue (and revenue growth) that far outpaces their other programs.
In 2019, ERAS took in $94 million in revenue - more than doubling its revenue from a decade before.
29
195
1K
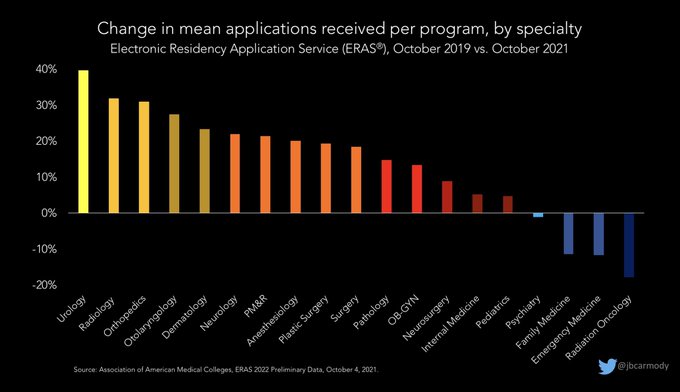
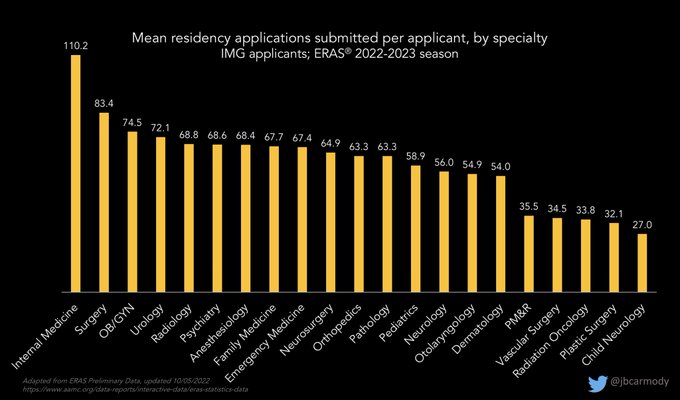
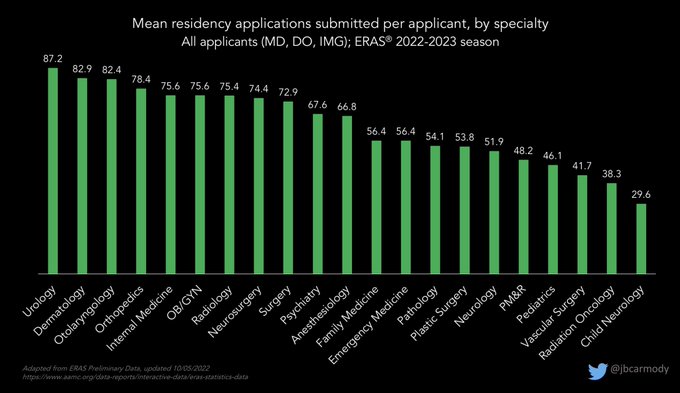
Preliminary data from ERAS are out… looks like another record-setting year.
The average number of applications received by residency programs is up in most specialties - in some cases, by 30-40% versus 2019.
#ApplicationFever
62
229
1K
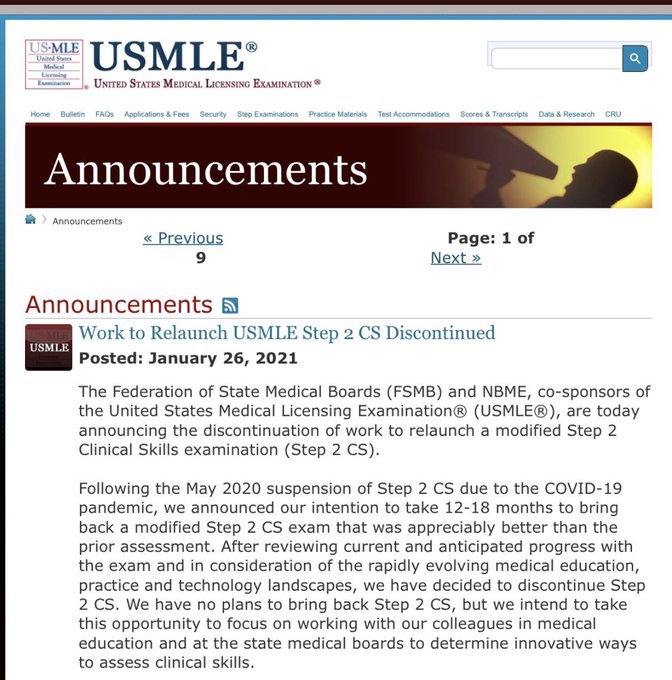
Well, all it took was a pandemic - but USMLE Step 2 CS is over.
(at least temporarily)
Official word should be coming from the USMLE later today.
#EndStep2CS
82
278
1K
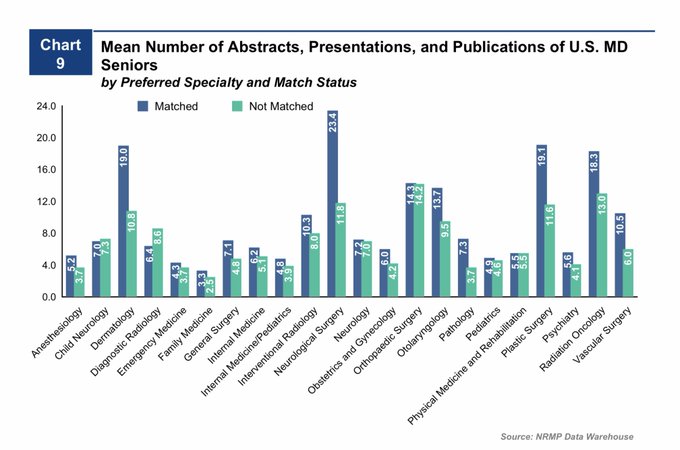
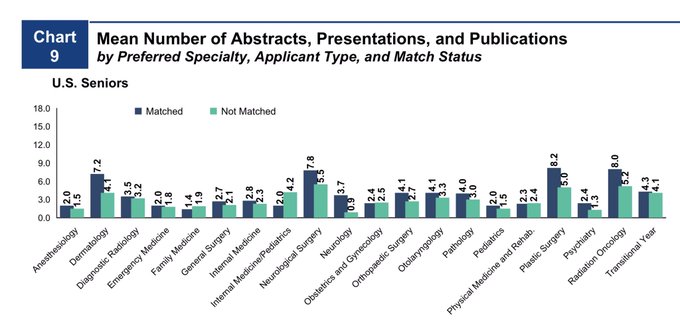
The research arms race for U.S. medical students
The average *unmatched* applicant in 2020 had more abstracts, presentations, and publications than the average *matched* applicant did in 2009.
(Data from
@TheNRMP
Charting Outcomes in the Match)
88
234
1K
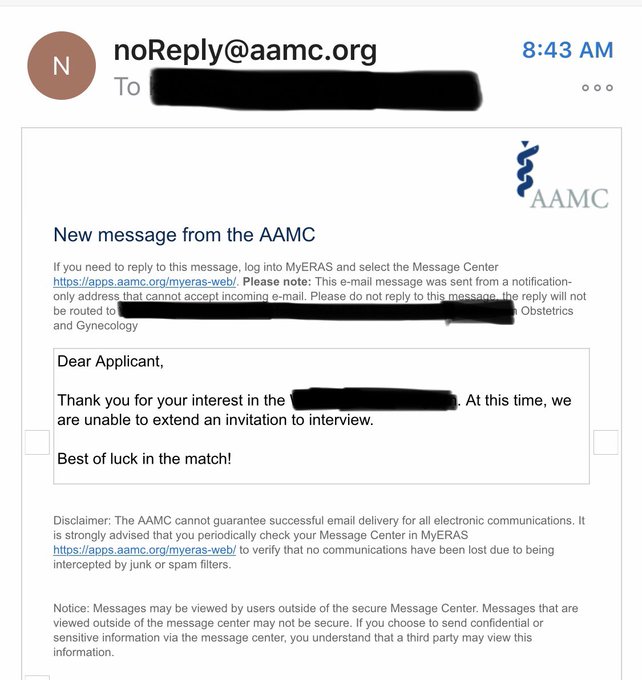
Show me a program that rejects an application in 15 minutes, and I’ll show you a program that needs to be honest with applicants about their ERAS filters.
I got a rejection 15 minutes into the season at 9:15 AM, probably an automatic reply to filtered out applications but that was fast.
#ERAS2023
50
13
543
17
111
1K
UPDATE:
Last week, a Nepali doctor filed a class action lawsuit against the National Board of Medical Examiners, alleging discrimination based upon national origin and requesting that invalidated USMLE scores be restored while examinees appeal.
Today, the NBME responded.
(🧵)
40
202
1K
Hang around
#MedTwitter
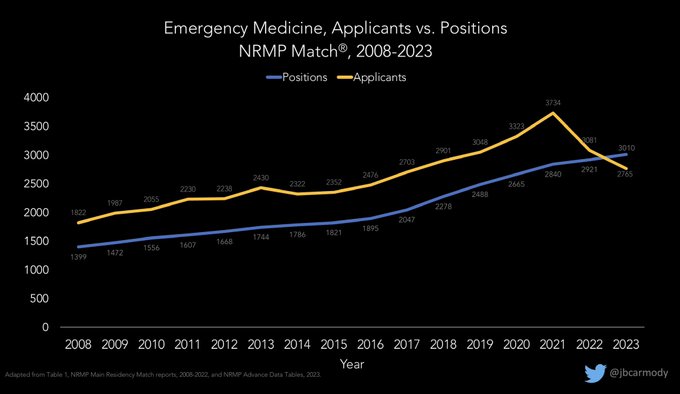
for a while, and you’ll find someone claiming that there aren’t enough residency positions for U.S. medical students, or that residency positions aren’t growing at the same rate as medical school graduates.
Trouble is, neither is true.
(a 🧵)
27
190
1K
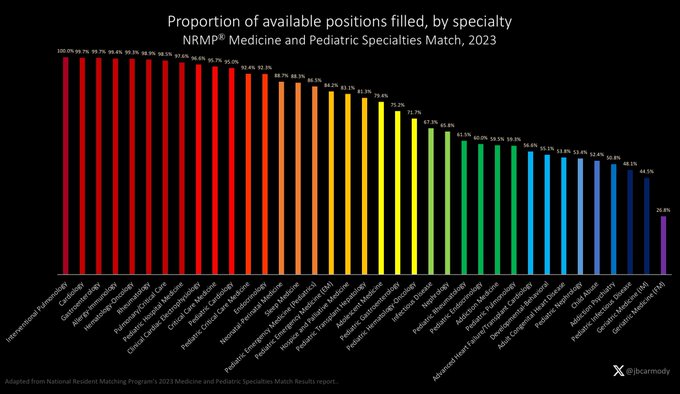
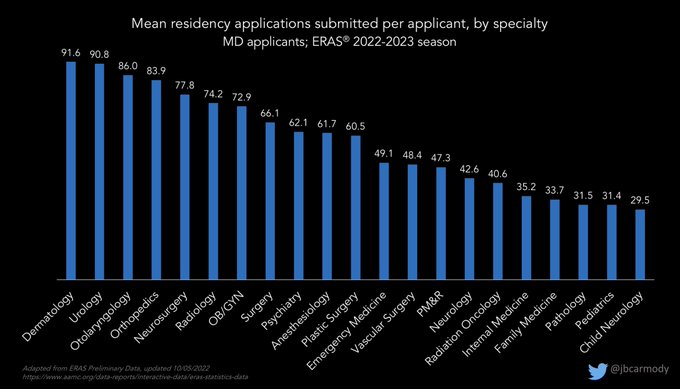
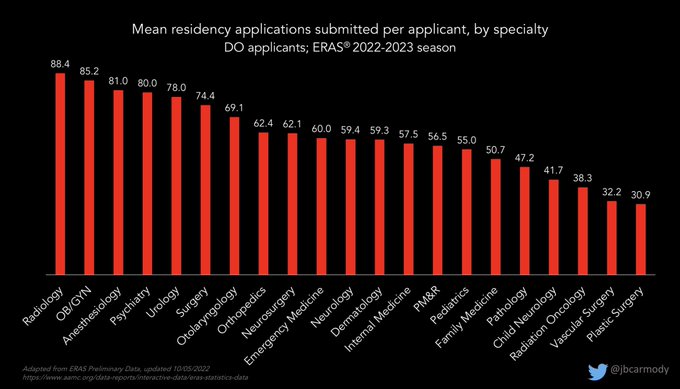
Preliminary data for this year’s residency application cycle are now available.
These figures won’t surprise anyone familiar with the contemporary application process… but if you’ve been out of the game for a while, some of the numbers will be eye-popping.
#ApplicationFever
58
186
996
This is a student’s worst nightmare.
You take
@TheUSMLE
… but somehow,
@PrometricGlobal
doesn’t record your test responses.
Some shameful stuff right here. A refund is necessary, but not sufficient.
87
79
954
ATTENTION PROGRAM DIRECTORS:
If you can reject an applicant within 43 minutes of ERAS opening, then you need to be more transparent about your filters.
(Save yourself some trouble; save the applicant $26.)
@JazmynShaw1
@DAndreaCeasar21
And for the record, this did happen today to a friend who’s applying to OBGYN.
8
6
70
22
106
930
Paying residents fairly is NOT incompatible with high-quality education.
21
49
875
I’ve gotten DMs asking “How could the USMLE prove they cheated? High scores alone don’t prove that!”
-and-
“How do I know my high score won’t be flagged as evidence of cheating just because of where I took the test?”
Lemme explain how I think these cheaters were caught.
(🧵)
30
137
768
@DGlaucomflecken
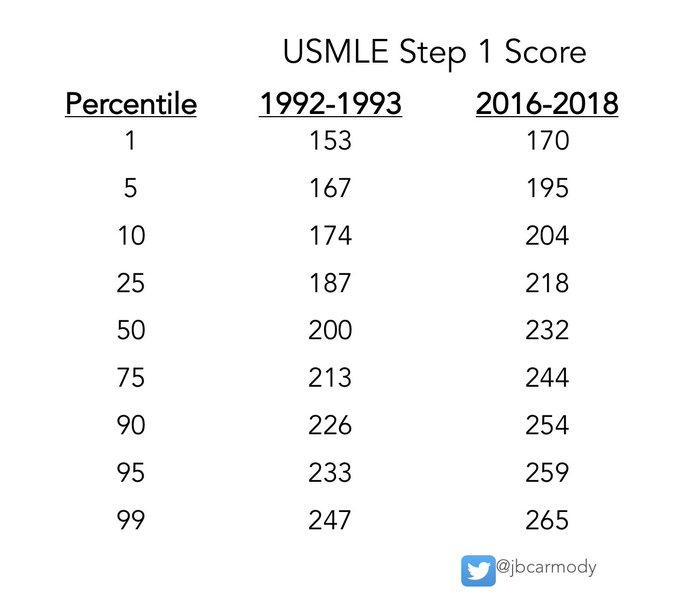
Seems like a good place to leave this.
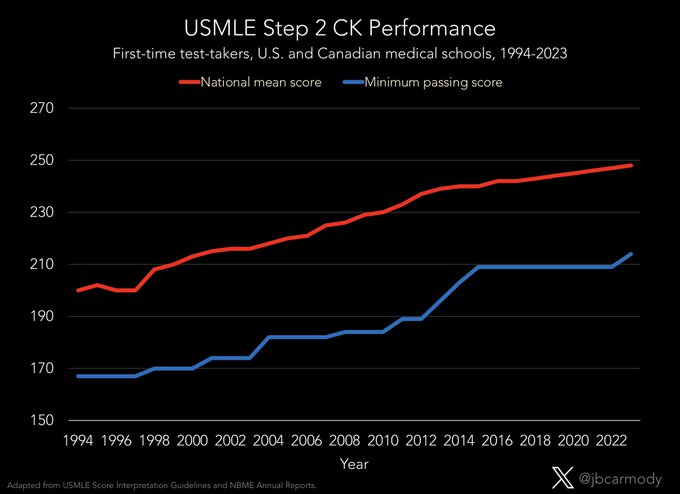
Today’s test-taker who scores at the median on USMLE Step 2 CK would have been in the 98th percentile if they’d taken the test 30 years ago.
2
70
767
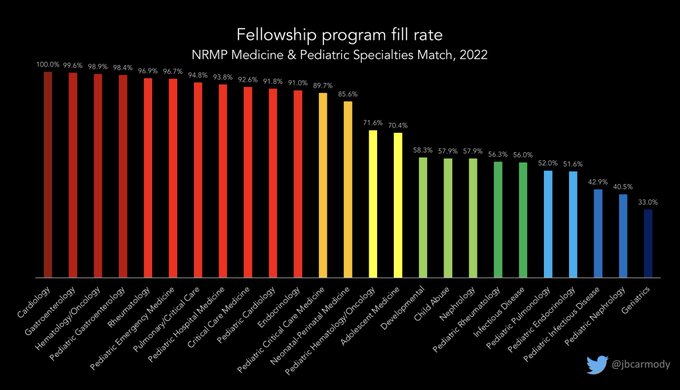
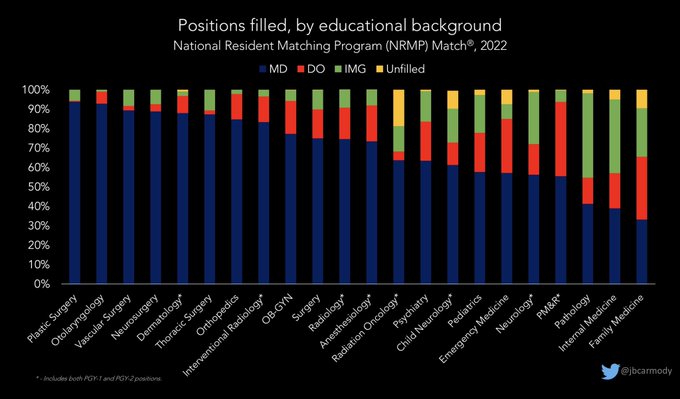
TODAY IS MATCH DAY!!!
Time for a quick 🧵 to explore the NRMP preliminary data.
Here’s how the specialties filled (or didn’t), by applicant educational background.
#Match2022
13
136
765
Big changes may be coming for internal medicine residency applicants in the 2024-2025 application cycle…
The
@AAIMOnline
is recommending:
-⬆️ preference signals from 7 to 15 (3 gold, 12 silver)
-capping interviews at 15
-no interviews before November 1
30
99
734
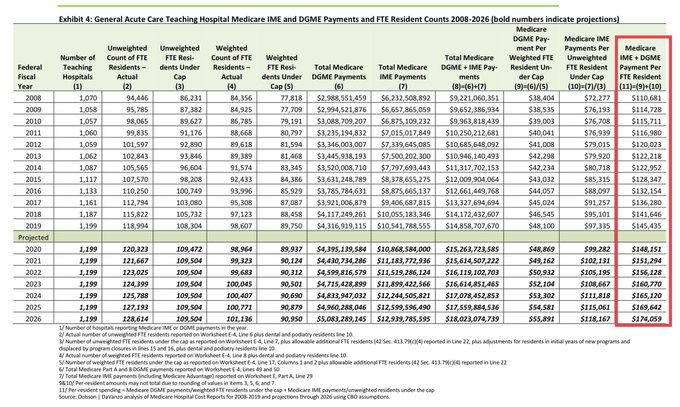
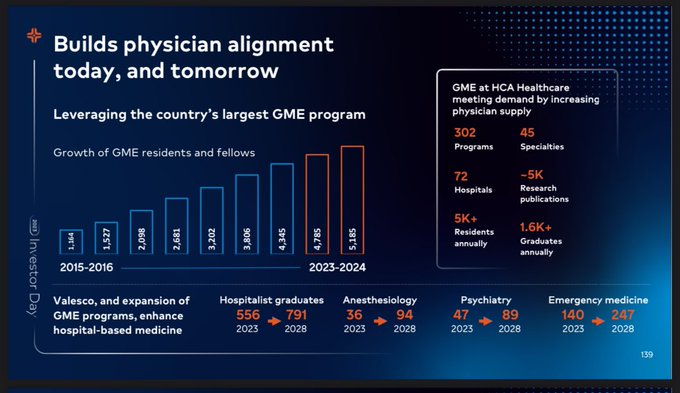
HCA is the nation’s largest for-profit hospital chain.
It’s also the
#1
sponsor of residency training programs in the U.S.
And HCA has **QUADRUPLED** the number of residents they train over the past decade.
(But yeah, tell me again how hospitals lose money training residents.)
31
107
721
The
@NBMEnow
has a task force to study whether high-stakes exams like the USMLE contribute to student burnout.
It sounds to me like their inclination is just to blame students for their lack of resiliency.
64
194
660
Succinct summary of what going tuition-free does for medical schools:
⬆️ selectivity
⬆️ U.S. News & World Report ranking
⬇️ % of students going into lower-paying specialties/primary care
“Relieving the burden of student loan repayment does nothing to address the link between wealth and medical school admissions in the United States.”
Read more from me and
@Jared_Boyce
via
@statnews
here:
9
71
277
28
146
641
Another Match Week has come and gone.
Time to break it down, Winners & Losers™️ style.
#MatchDay2022
31
134
625
Your move,
@NBOME
.
Today, the USMLE Program is announcing the discontinuation of work to relaunch a modified Step 2 Clinical Skills examination (Step 2 CS). Read the full statement here
#MedTwitter
#MedEd
91
955
3K
22
97
614