Vijay Iyer PhD
@vijayiyer312
Followers
4K
Following
29K
Media
128
Statuses
12K
Patient advocating science for #mecfs & #dysautonomia (incl via #longcovid & #postvac).👷🏾♂️Support #neuroscience users & use cases of @MATLAB. Tweets my own.
Boston, MA
Joined December 2017
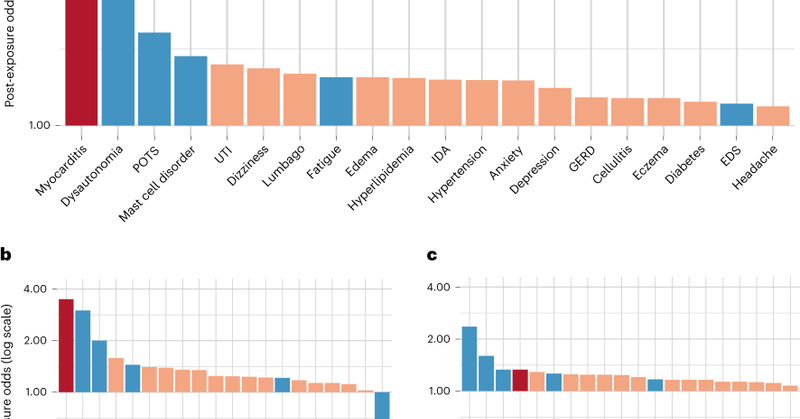
I can sort of understand this, but myocarditis is very rare and tends to resolve; while the vax does confer long term immunity beyond just antibodies. That said I'm also close to 'beyond the pale' wrt the C19 vax given it triggers or hastens POTS at ~100x rate of myocarditis.
I can’t imagine prescribing a medication for a cold that might cause my patients myocarditis. It’s totally beyond the pale.
1
0
3
RT @Poisson_dart: @orphcorp Tbh the person who responds negatively to a contradiction being pointed out (a pro-cognitive behavior that shou….
0
3
0
RT @dacolon: Neurons are hungry for energy, and carry their own batteries. Excited to share our latest study, on the use of glycogen by ne….
news.yale.edu
A new Yale study reveals that neurons store their own sugar reserves that kick in to keep the brain functioning during metabolic stress.
0
20
0
RT @wtogami: I have been substantially disabled by Long COVID since 2022. Received Pemgarda infusion July 17th, 2025 after reading a few an….
0
74
0
RT @ruimcosta: Together we go farther. Thanks to a partnership with @ASAP_Research and @MichaelJFoxOrg, the @AllenInstitute's ABC Atlas no….
0
16
0
While I disagreed with how Dr. Ladapo spoke exclusively to vaccine-triggered conditions during the pandemic, I welcome his broader view here. #longvax is too big a clue* to lose to taboo! (and vice versa). *into #longcovid.
0
0
1
RT @jacobbiasetti: I’m 22 years old. I’ve been completely bedridden for almost 2 years now with MECFS. It was triggered by a stomach bug.….
0
209
0
RT @Michael_J_Black: @OHilliges It is great that you're posting - the more attention the better. I have multiple friends whose lives have b….
0
2
0
RT @OHilliges: Sadly, I am no longer a professor at ETH (@eth_en) due to very severe #longCovid and #MECFS.
ethrat.ch
Der ETH-Rat hat an seiner Sitzung vom 9./10. Juli 2025 Kenntnis genommen vom Rücktritt von Vanessa Wood als Vizepräsidentin der ETH Zürich. Sie verlässt die Schulleitung per Ende Dezember 2025 und...
0
143
0
While I see lots of good things from #neuroimaging (with human MRI etc), it's also clear to me much of public & medicine doesn't know how far micro-scale #neuroscience has come (which is mostly animal).
Not studying animal models would halt basic neuroscience. We don’t have good AI models of animal brains to study and we can’t study human brains at single spike single neuron resolution. Studying the brain using fMRI is like studying the economy from a telescope on the moon.
0
0
0
RT @dysclinic: Here is my takeaway from interacting with my friends and colleagues - some of the best autonomic specialists in the world -….
0
18
0
RT @ElianaUku: The impossible happened. I recovered from bedbound, to housebound, and now I'd consider myself mild on the #longcovid #mecfs….
0
59
0
Good points, though it has to be more than the 'reach of care'. Longitudinal tracking could become a major new 'source of discovery'.
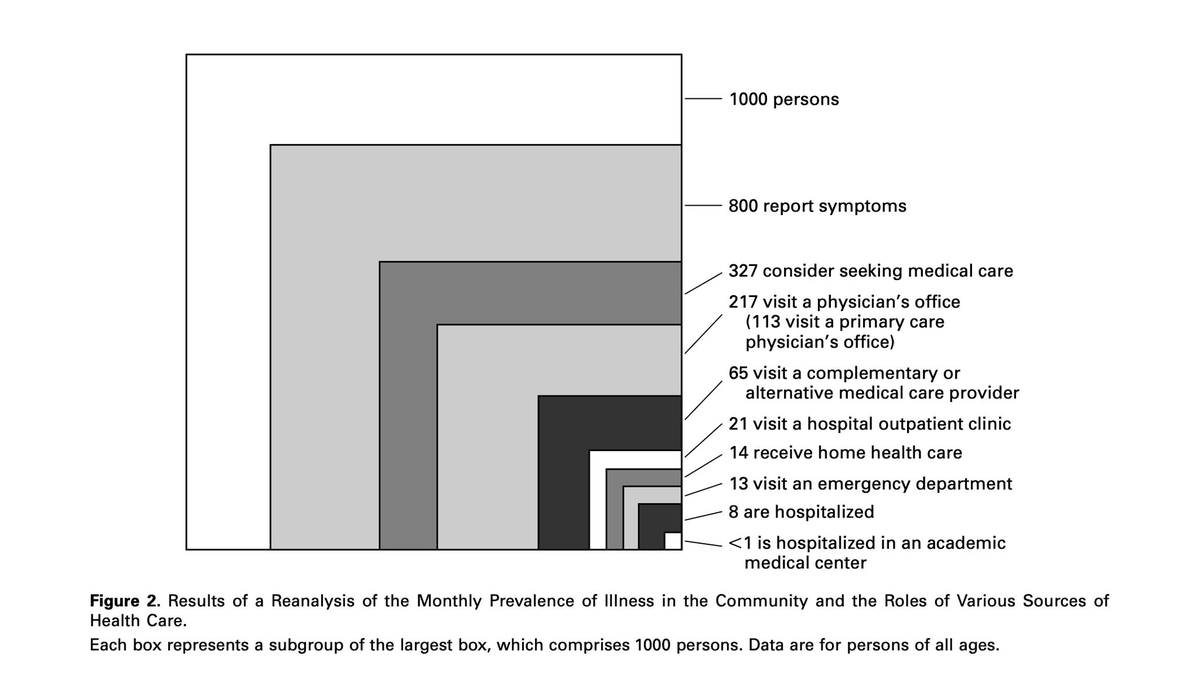
this diagram is one of the most important in medicine. published over two decades ago, "The Ecology of Medical Care" captured a persistent truth:.- of every 1000 people, 800 report symptoms each month. - 327 consider seeking care. 217 actually do. - 8 are hospitalized. - fewer
0
0
0
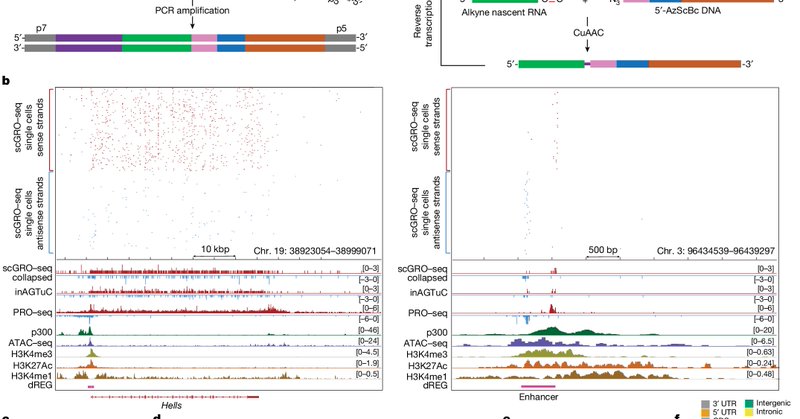
RT @ndtippens: What if we could quantify RNA synthesis directly? My colleague @DigbijayMahat has recently achieved this feat at single-cel….
nature.com
Nature - Nascent transcription in genes and enhancers genome-wide at the single-cell level is quantified using global run-on and sequencing (GRO–seq) with click chemistry.
0
7
0
Same with "stress". Lewis Thomas pushed back on demonization of stress back in the 70s & 80s with a quote to effect of "stress is life". I'm trying to relocate source of this spot-on point.
One of the biggest mistakes we’ve made is to demonize anxiety. Anxiety is the ontological affect par excellence. It brings us face to face with nothingness. It opens us up to the possibility of reorienting in a topsy-turvy world. We cannot think without anxiety.
0
0
0
Very interesting work! Though I would scope the description to what's been found: a neural substrate for prolonged/delayed pain sensitivity. The amygdala & insular cortex have not been so finely mapped or fully understood that projections thereto imply "affective".
New paper out in @PNASNews. Thalamic CGRP neurons form a spinothalamic pain pathway relaying pain signal to the amygdala & insular, but not sensory cortex to encode the affective dimension of pain. Huge congrats to first author @SJ_J_Kang_24 & coauthors.
0
0
1
RT @StavrosZanos: @itchdoctor Read your paper when it came out and I agree 100%. I would argue that animal models (not only mice) are still….
0
1
0
I don't understand VCs obviously. They quote a passage saying the brain has a bunch of unconscious modules driving us and then tweet about "the brain" as if those don't exist. Apparently what drives us isn't investable 🤷🏽.
The more I study neuroscience, the less I’m convinced that the human brain is meaningfully different than an LLM. Recent studies show that our brain often decides to take an action before we’re even conscious of the decision. And then we come up with rationale afterwards to
0
0
0
RT @manorlaboratory: My lab’s 5-year NIH R01 grant, awarded to study gene therapy for hearing loss, was abruptly terminated. I want to shar….
0
2K
0