Helbert Rondon, MD, MS, FACP, FASN, FNKF
@NephroMD
Followers
6,693
Following
968
Media
441
Statuses
5,633
Nephrologist @UPMC l Professor of Medicine @PittDeptofMed l Fellowship PD @Pittrenal | Tweets/retweets are my own #Hyponatremia
Pittsburgh, PA
Joined April 2009
Don't wanna be here?
Send us removal request.
Explore trending content on Musk Viewer
Fenerbahçe
• 635770 Tweets
#RafahOnFire
• 374417 Tweets
Memorial Day
• 180011 Tweets
Şampiyon Galatasaray
• 126671 Tweets
#GazzeKanGölü
• 109264 Tweets
Admin
• 99258 Tweets
#مجزره_رفح
• 78172 Tweets
Ali Koç
• 63306 Tweets
خيام النازحين
• 53408 Tweets
Allah'ım
• 49412 Tweets
İsrail
• 45373 Tweets
#رفح_الان
• 35072 Tweets
Fermin
• 34801 Tweets
Ankaragücü
• 33759 Tweets
Ronaldinho
• 27994 Tweets
Ludmilla
• 25667 Tweets
Ergin Ataman
• 24137 Tweets
Trabzon
• 22771 Tweets
Ya Kahhar
• 20347 Tweets
Larson
• 18845 Tweets
ドラクエの日
• 17903 Tweets
Amaral
• 13202 Tweets
東京都知事選
• 12596 Tweets
Ya Rabbi
• 12394 Tweets
Moisés
• 10913 Tweets
Rodrigues
• 10008 Tweets
Last Seen Profiles
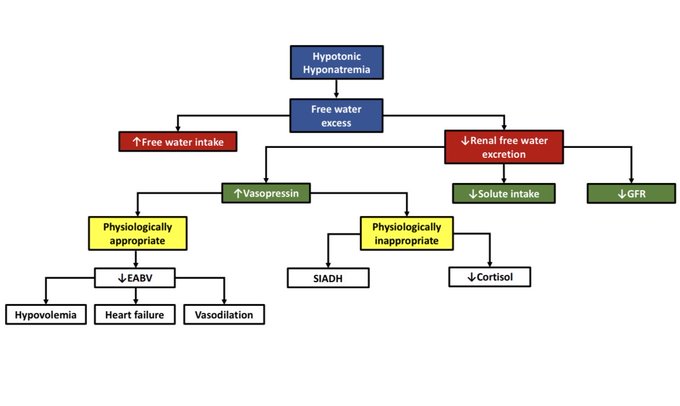
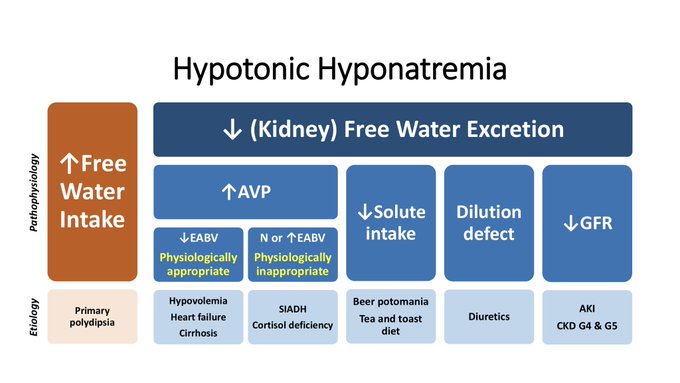
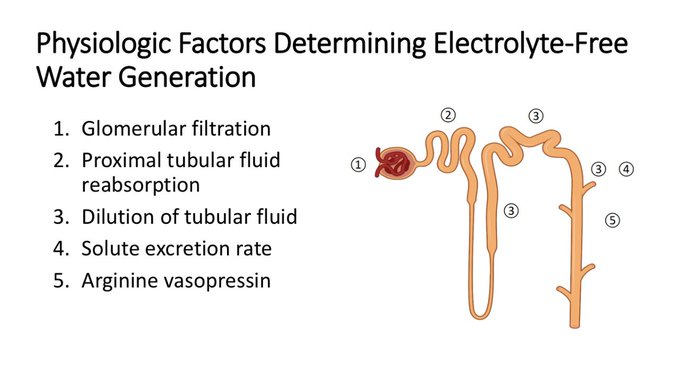
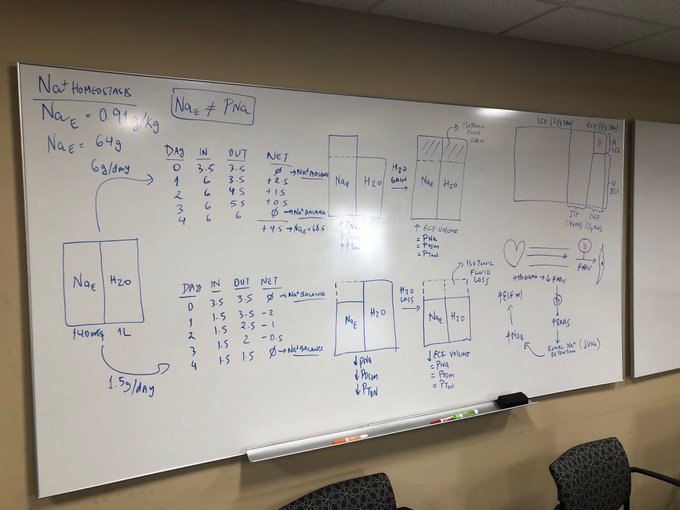
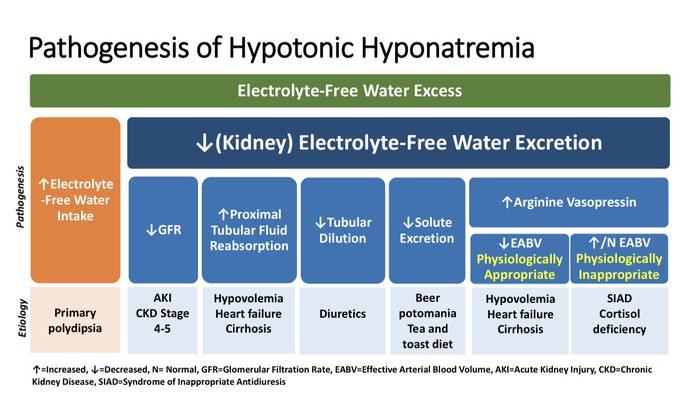
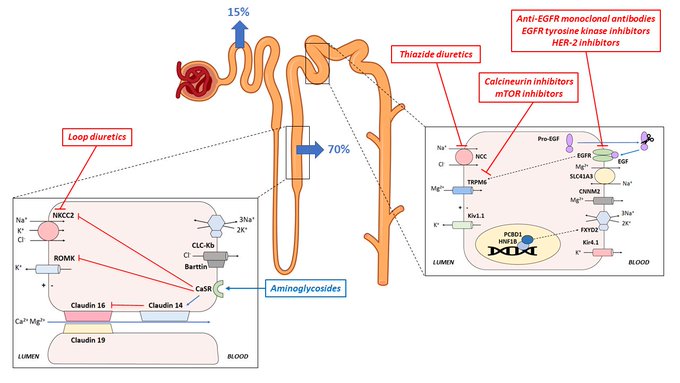
Updating my pathophysiology of hyponatremia slide for a talk. Thanks
@swissnephro
for the art inspiration.
8
78
367
Time for a
#tweetorial
on “Desalination” in SIADH. Why normal saline (NaCl 0.9%) makes the
#hyponatremia
from SIADH worse?
11
86
198
Time for another
#tweetorial
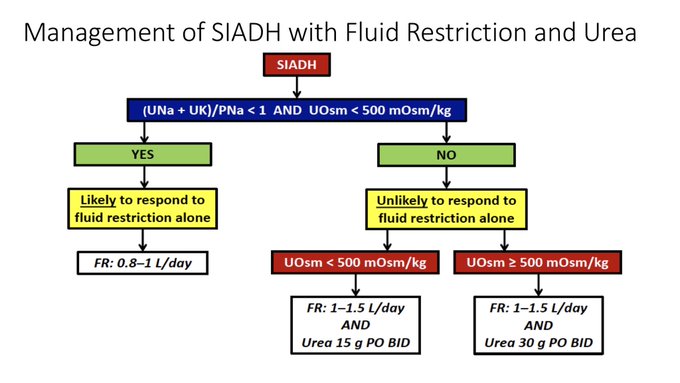
on fluid restriction in
#hyponatremia
from SIADH. Is there a way to predict which patients with SIADH will respond to fluid restriction?
8
86
198
Our manuscript “Hyponatremia Demystified: Integrating Physiology to Shape Clinical Practice” in collaboration w/
@ChristCrain
@bdubNephro
@priti899
is now available online
@ackdonline
@PITTRenal
@pittkidneyctr
@ClinNeuroEndo
@MDACC_RenalSec
#hyponatremia
9
58
176
I developed video lectures as a part of a
#FlippedClassroom
on
#hyponatremia
for our IM residents. I am going to be posting one of those videos every week. This is Lecture
#1
: Basic Physiology of Sodium/ECF Volume Homeostasis.
12
61
164
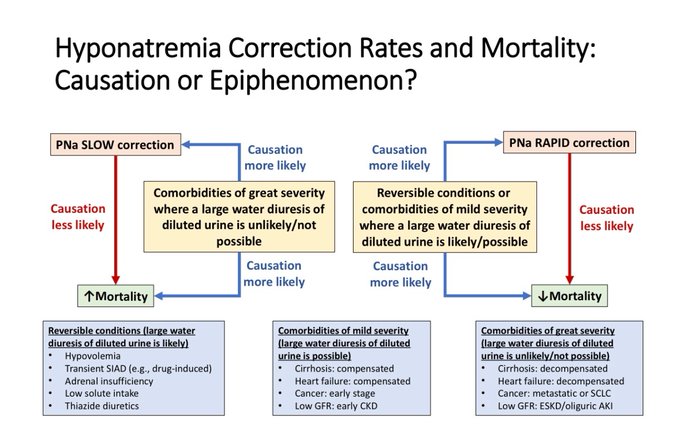
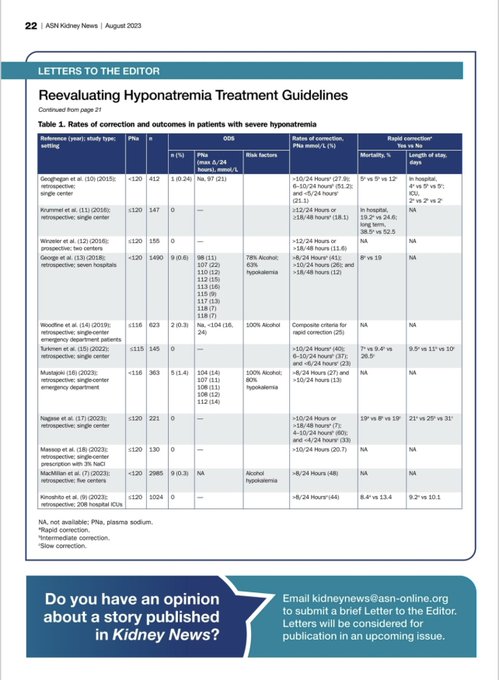
It is implausible that a few mmol/L change in PNa is responsible for fatalities. It is far more likely that underlying comorbidities and their severity is responsible for mortality observed.
#hyponatremia
4
55
159
My review on
@CJASN
on “Therapeutic Relowering of Plasma Sodium after Overly Rapid Correction of Hyponatremia: What is the Evidence?”
#hyponatremia
is now available:
6
63
147
My fellows gave me this gift. Love it! Thanks
@AravindCheruku1
@kkalra_22
@siddverma96
@ripudamanmunjal
@drnawras1986
@IvyM808
7
3
148
@AvrahamCooperMD
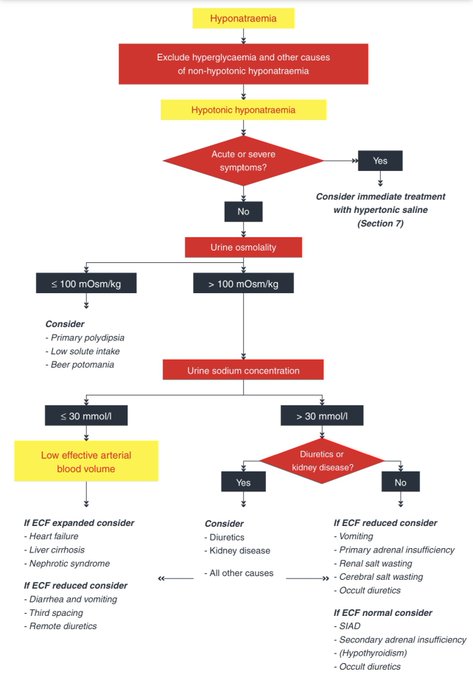
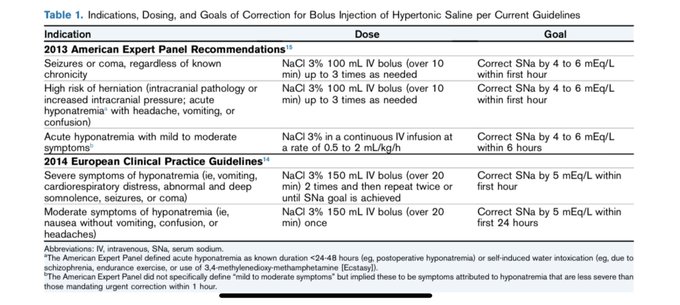
This is the traditional algorithm that hopefully most physicians are moving away from. Recommend instead a physiological approach as shown in the 2014 European practice guidelines.
5
27
142
@MunerMohamed1
There is no way this patient is not volume depleted from glucosuria-induced osmotic diuresis but with much more urinary water than sodium losses. His corrected Na is actually 187 and his total body K is in the tank. I would start with LR + KCl
3
2
140
24 specialists from 20 institutions across 🌎 just published a review in
@CJASN
urging caution & adherence to
#hyponatremia
correction guidelines. Motivated by concerns over uncritical acceptance of a recent study & its editorial
7
51
119
1/ I find the over reliance on the Adrogue-Madias (AM) formula to predict SNa changes after infusion of a specific IV fluid astounding.
#hyponatremia
tweetorial
2
51
117
First official day as Nephrology Fellowship Program Director
@PITTRenal
. Will do our best to continue the legacy of
@jamierj2
. Big shoes to fill!
15
4
110
Honored and excited to become part of the editorial board of
@CJASN
. Thanks
@rajmehrotra1122
for the opportunity.
16
3
105
Happy to share that our review of “
#Hyponatremia
in Cirrhosis” in collaboration with all-things-liver aficionado
@VelezNephHepato
published in Clinics in Liver Disease is now available online
#livertwitter
8
42
97
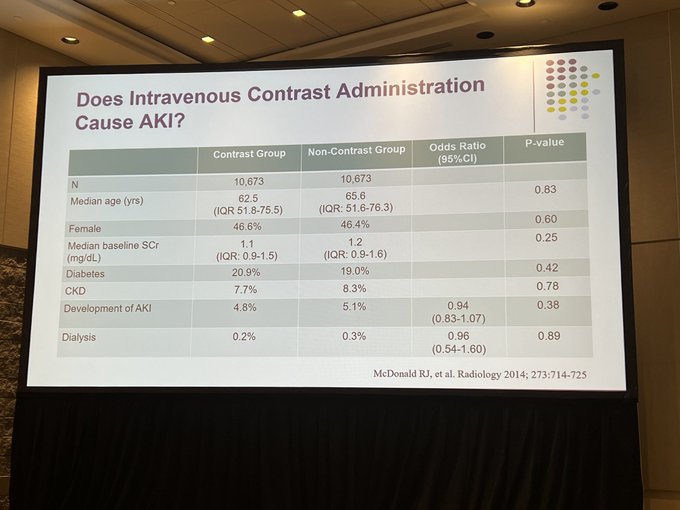
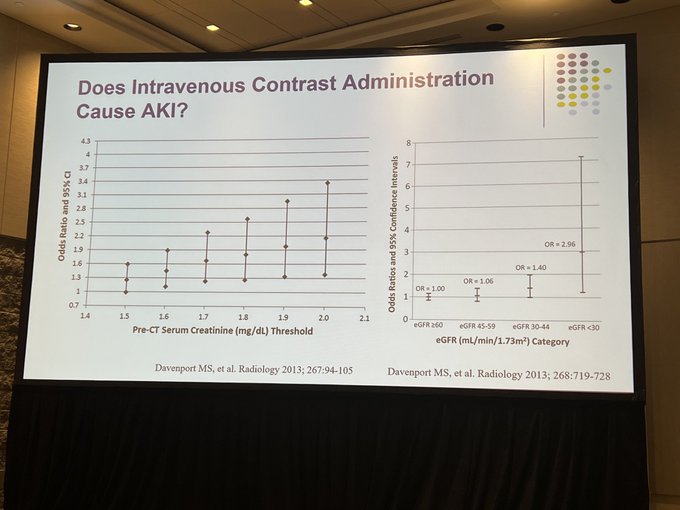
Does contrast associated AKI exist? risk is less these days but, yes, it does
@PaulPalevsky
#KidneyWk
3
24
88
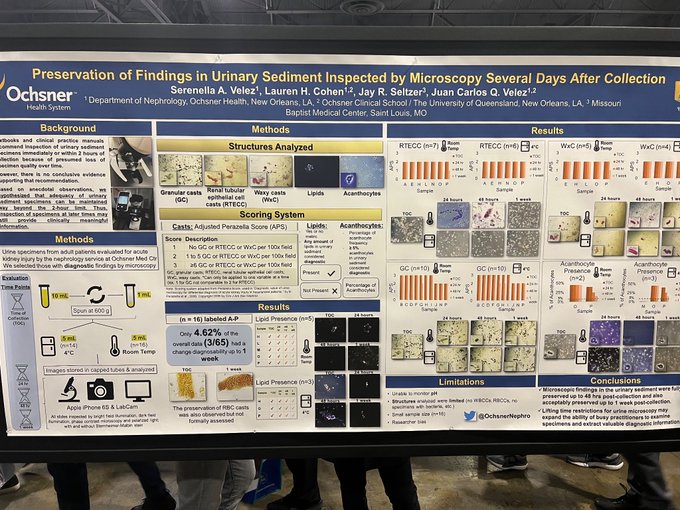
SA-PO1035- Leaving a urine sample for a week, and at a room temperature does not alter the microscopic findings in urine sediments. Important findings from
@serenellaavelez
and
@VelezNephHepato
7
25
92
My 3rd video lecture of the
#ElectrolyteClub
series on
#hyponatremia
. Lecture 3: Pathophysiology and Etiology of Hypotonic Hyponatremia - Part 1.
1
21
83
Our new study "Osmotic Demyelination Syndrome Following Correction of Hyponatremia by ≤10 mEq/L per day" in collaboration with Richard Sterns and my former fellow , Srijan Tandukar
@Tandukar702
@PITTrenal
is now available in
@ASNKidney360
#hyponatremia
1
32
81
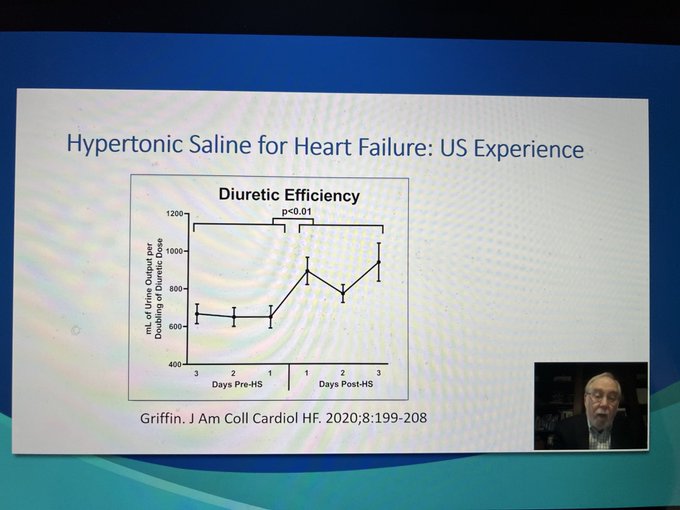
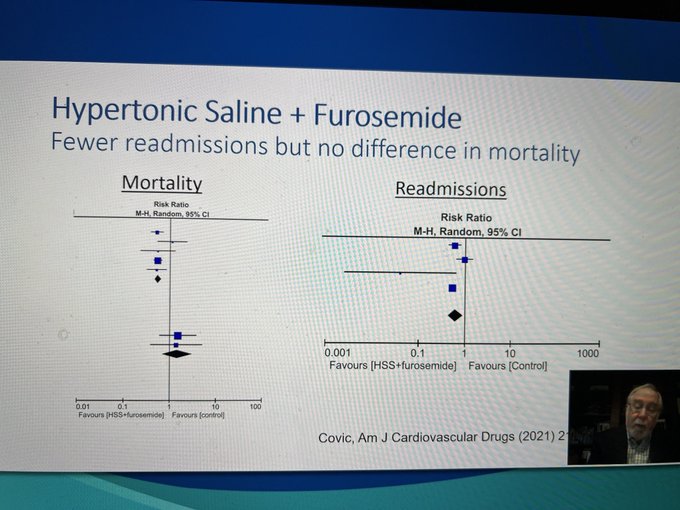
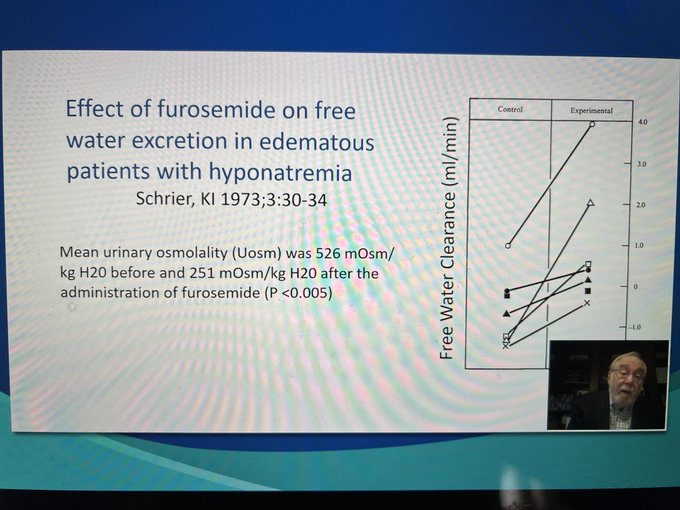
Hypertonic saline and furosemide seem to be an effective therapy for hyponatremia in diuretic resistance heart failure - Richard Sterns
#KidneyWk
@ASNKidney
3
9
82
Our review on “Diagnostic and Therapeutic Strategies to Severe Hyponatremia in the Intensive Care Unit” is now available online at the Journal of Intensive Care Medicine
#hyponatremia
3
25
87
Starting my vacation to
@peru
🇵🇪to visit
#machupicchu
. Packing the obligatory reading materials for the flight.
11
9
76
Furosemide works essentially as a “vasopressin antagonist” - Richard Sterns
#KidneyWk
@ASNKidney
1
22
70
Our latest review of "Hyponatremia in the Cancer Patient" published in the October issue of
@Kidney_Int
@bdubNephro
@kdjhaveri
2
25
67
Our recent review on “Hypomagnesemia in the cancer patient” just published in
@ASNKidney360
@bdubNephro
@kdjhaveri
This Review Article by Biruh T. Workeneh, Nupur N. Uppal,
@kdjhaveri
and
@NephroMD
summarizes magnesium physiology and highlights the mechanisms underlying magnesium disturbances due to cancer and cancer treatment.
@MDAndersonNews
@HofNorthwellDOM
@UPMC
0
30
81
2
19
67
3/That is why Rick Sterns and I decided to write an editorial about this paper for
@KidneyNews
1
9
64
@Maximal_Change
@EM_RESUS
Yes! One of the common mistakes of management of hyperkalemia is that providers give 1 amp of calcium gluconate and then they forget about the wide QRS. You have to keep giving calcium every 5 min with until QRS narrows.
1
15
61
Honored to be invited to speak on
#hyponatremia
and SIAD at the 2023 American College of Physicians
@ACPinternists
national meeting in San Diego in April.
#ACP2023
3
3
66
@ganti_anita
@PittGIM
@CaseyMcQuadeMD
@mgsimonson1
This is actually my slide and I use it to show that this algorithm is awful and should not be used
9
0
62
Second video of the
#ElectrolyteClub
series on
#hyponatremia
. Lecture
#2
: Basic Physiology of Water/Plasma Tonicity Homeostasis.
4
24
56
Thanks to
@ASNKidney
and the
#KidneyWk
program committee for the invitation to speak on
#hyponatremia
in Philly this November. Looking forward to the discussion and another fantastic meeting.
4
0
60
Two letters (and our response) about our
@KidneyNews
May issue commentary on the controversial study regarding ODS in
#hyponatremia
are now available online.
1
23
61
Out paper of “Hyponatremia in the cancer patient” with
@bdubNephro
and
@kdjhaveri
is now available online
3
9
57
Our review in collaboration with Richard Sterns titled "Hypertonic Saline for Hyponatremia: Meeting Goals and Avoiding Harm" is now available
@AJKDonline
#hyponatremia
4
24
56
A good and succinct review on
#hyponatremia
in the last issue of NephSAP on Electrolytes and Acid Base Disorders However, sad to see they are still recommending the classic diagnostic algorithm using volume assessment
3
10
55
@kidney_boy
Ha! the problem is that Google university medical school is not graduating enough doctors to combat this epidemic
0
5
41
Our manuscript on "Serum Sodium Trajectory during AKI and Mortality Risk" in collaboration with
@JonathanNefro
@kianoushbk
and other colleagues is now available online
@JournalofNeph
4
12
51
Pre-conference course on Fluid, Electrolytes and Acid-Base disorders completed - Faculty: Biff Palmer Susie Hu
@NephRodby
#NKFClinicals
2
4
52
Lecture
#5
of the
#ElectrolyteClub
series on
#hyponatremia
: "Pathophysiology and Etiology of Hypotonic Hyponatremia - Part 3"
0
11
50