ERS publications
@ERSpublications
Followers
30,479
Following
308
Media
3,780
Statuses
15,472
European Respiratory Journal, European Respiratory Review, ERJ Open Research, Breathe, the ERS Monograph and ERS Handbooks, and European Lung White Book
www.ersjournals.com
Joined November 2011
Don't wanna be here?
Send us removal request.
Explore trending content on Musk Viewer
Iran
• 1410417 Tweets
ايران
• 658434 Tweets
#سیدالشهدای_خدمت
• 103652 Tweets
HITCHHIKER
• 36582 Tweets
THANK YOU PAGTATAG
• 26827 Tweets
COMING OF AGE DAY
• 26477 Tweets
なにわ男子
• 24407 Tweets
#LokSabhaElctions2024
• 21802 Tweets
VisiPRABOWO RakyatSEJAHTERA
• 21134 Tweets
Lied to you
• 21116 Tweets
KitaKOMPAK KitaMAJU
• 20273 Tweets
Happy New Week
• 18338 Tweets
Gcinile
• 17180 Tweets
交通系IC
• 14146 Tweets
#MondayMotivation
• 14072 Tweets
衆院・政倫審
• 12261 Tweets
自民党裏金事件めぐり
• 10972 Tweets
RIDDLE
• 10612 Tweets
Last Seen Profiles
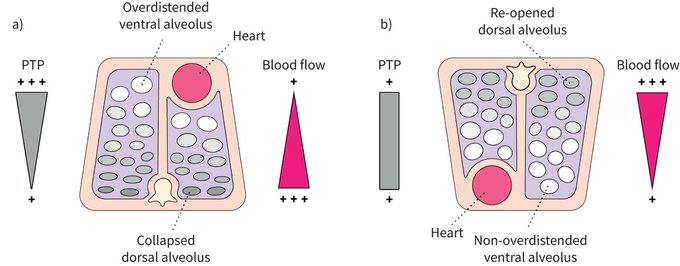
In intubated ARDS patients, prone positioning reduces mortality. On spontaneously breathing patients, oxygenation improved during awake prone positioning. Relevant data on clinical outcomes are expected, especially on
#COVID19
patients.
0
88
170
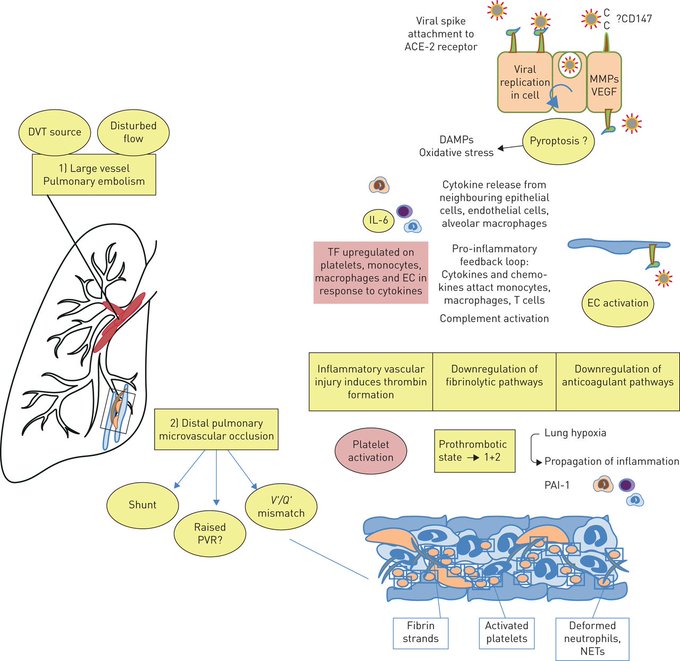
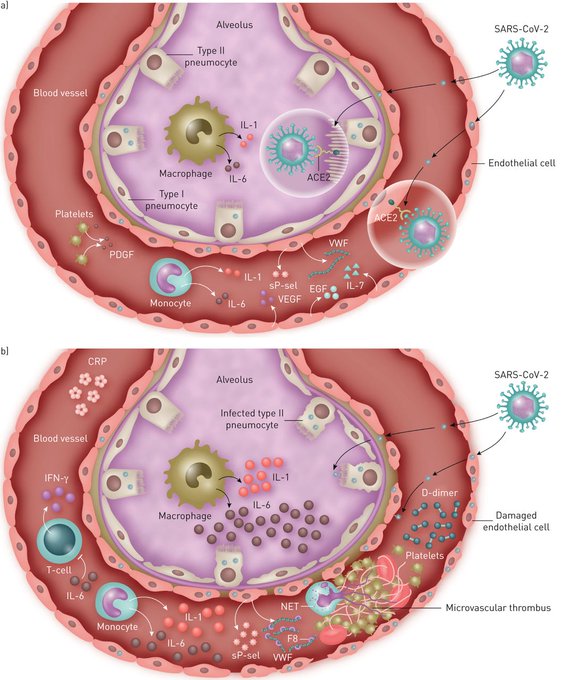
Pulmonary thrombosis appears to be common in
#COVID19
pneumonia and takes two forms, proximal pulmonary emboli and/or distal thrombosis. The possible mechanisms and clinical implications are discussed.
0
89
167
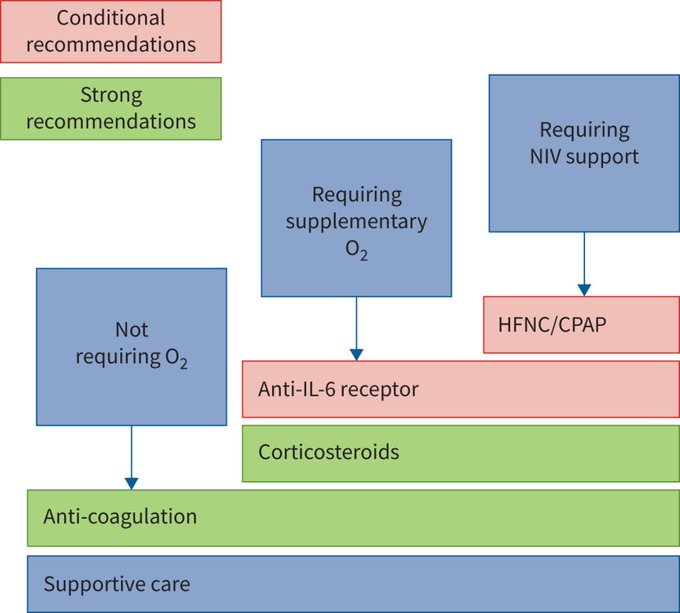
The ERS guidelines for the management of
#COVID19
make recommendations in favour of corticosteroids, thromboprophylaxis, anti-IL-6 and noninvasive ventilatory support. These guidelines will be regularly updated as further evidence becomes available.
0
81
136
Pneumomediastinum in severe
#COVID19
presentations could be due to a lung parenchymal retractive process generated by intense inflammation as in acute exacerbation of idiopathic pulmonary fibrosis or MDA-5 acute interstitial lung disease
1
47
128
Corticosteroids and anti-IL-6 receptor antagonist monoclonal antibodies reduce mortality in hospitalised patients with
#COVID19
3
60
127
In discharged survivors with
#COVID19
, impairment of diffusion capacity is the most common abnormality of lung function, followed by restrictive ventilatory defects, which are both associated with the severity of the disease
0
75
122
A complication of
#COVID19
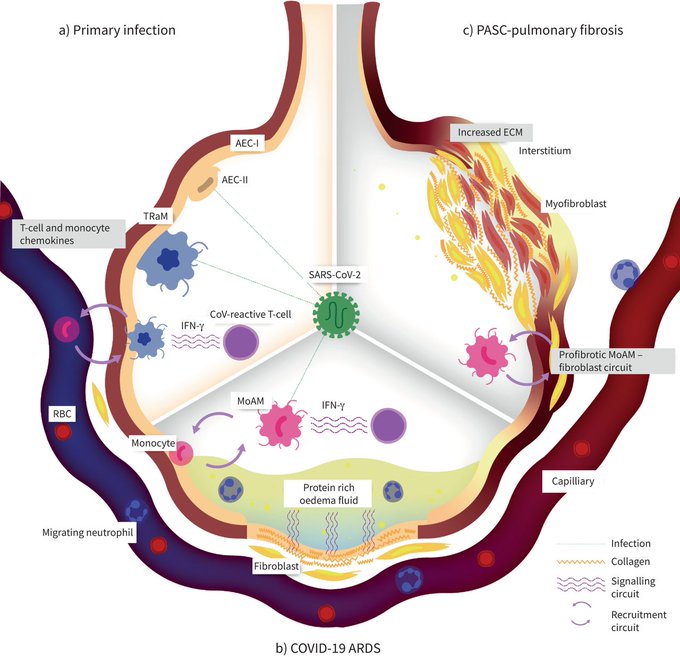
, PASC-pulmonary fibrosis, has potential to become a global respiratory health crisis. Dedicated surveillance, mechanistic understanding and clinical and research efforts are needed to confront this emerging sequela of COVID-19.
0
59
106
#COVID19
pulmonary sequelae are unknown. The Swiss COVID-19 lung study reports on initial follow-up findings. Severe or critical COVID-19 was associated with significant functional impairment and radiological abnormalities after 4 months.
1
50
100
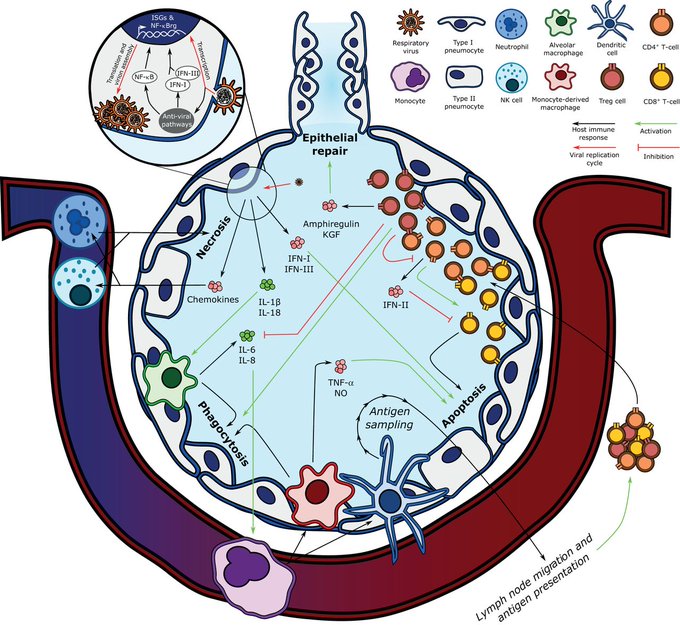
Review of viral ARDS pathogenesis, how it informs evolving models of
#COVID19
, and how hallmarks of ageing explain the age-related morbidity and mortality of severe COVID-19
1
48
100
Breathlessness is a major cause of suffering across populations that relates strongly to increased healthcare utilisation and major adverse health including shorter survival
@MJJohnson_HYMS
0
40
97
Hypercytokinaemic immune dysregulation in
#COVID19
is known as cytokine storm syndrome. Interleukin-6 levels ≥80 pg/mL predict an increased risk of respiratory failure and death, and immunomodulatory therapy is an area of urgent investigation.
0
49
96
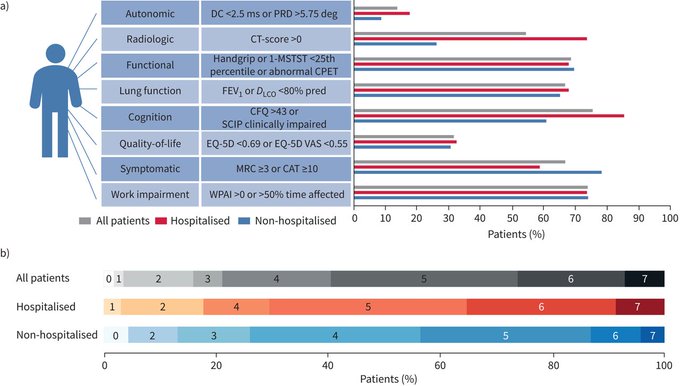
3 months post-COVID-19, most patients have at least one organ function impairment. All patients have some degree of cognitive impairment and abnormal dyspnoea symptom scores. Abnormal HRCT and impaired DLCO are predominately found in inpatients.
#longCOVID
1
49
92
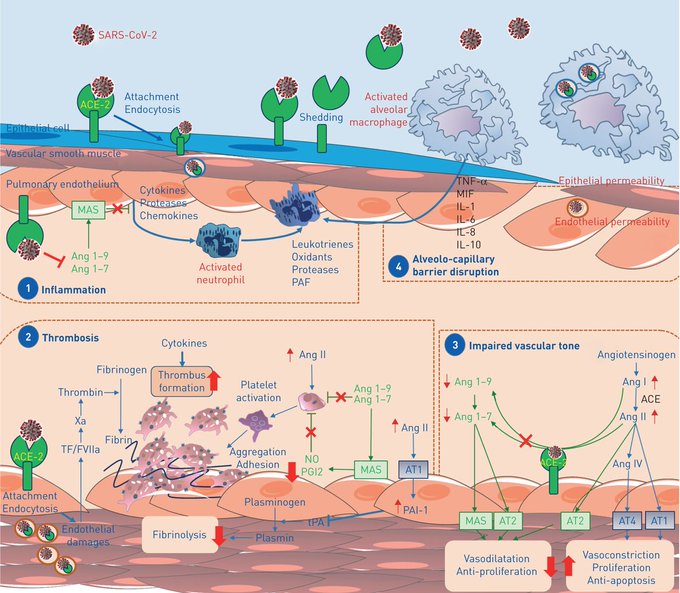
Endothelial cell dysfunction and impaired microcirculatory function contribute markedly to life-threatening complications of
#COVID19
, such as venous thromboembolic disease and multiple organ involvement
0
56
89
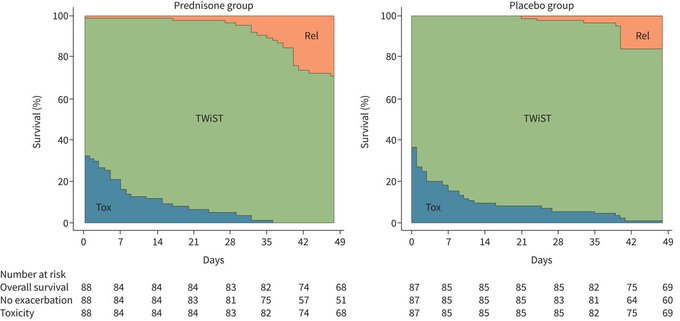
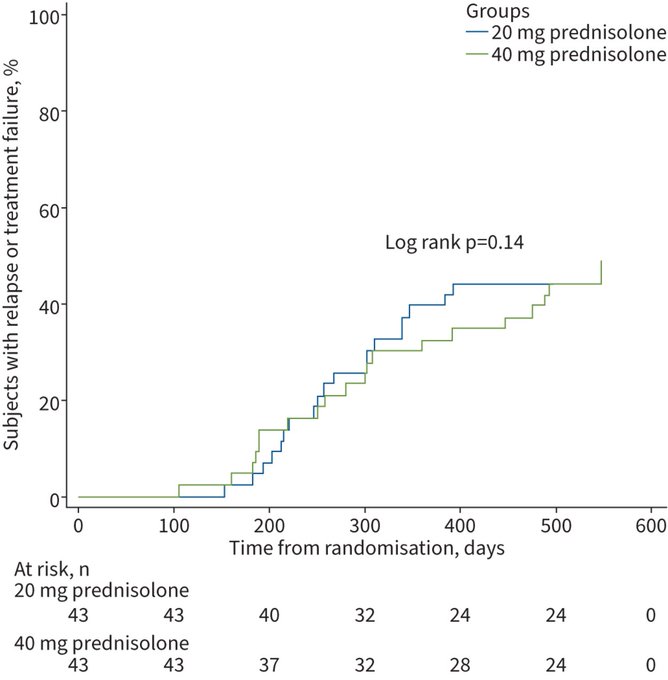
High-dose prednisolone may not be superior to a low-dose 6-week regimen in improving clinical, physiological and radiological outcomes, or health-related quality of life, in patients with symptomatic post-
#COVID19
diffuse parenchymal lung abnormalities
1
58
88
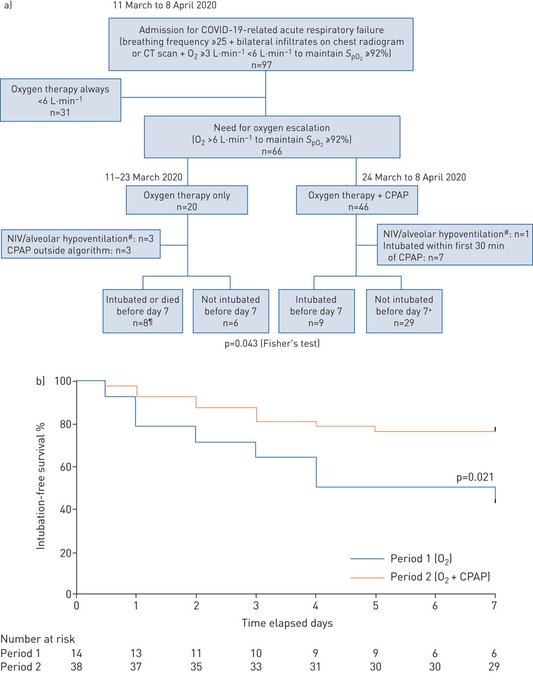
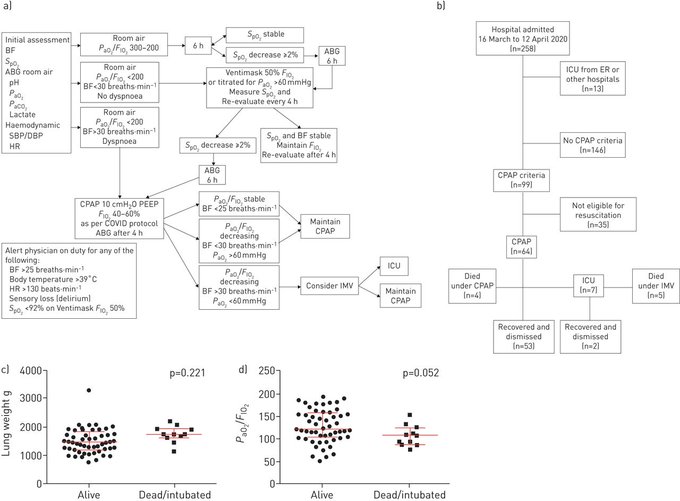
#COVID19
pneumonia can be life-threatening. Given the unprecedented burden placed on ICU resources by the epidemic, avoiding intubation is a major issue. This study suggests that CPAP can achieve this objective.
2
53
88
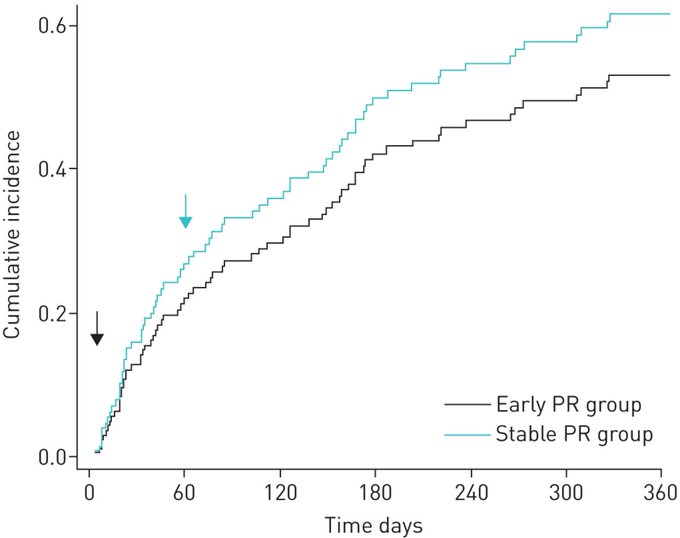
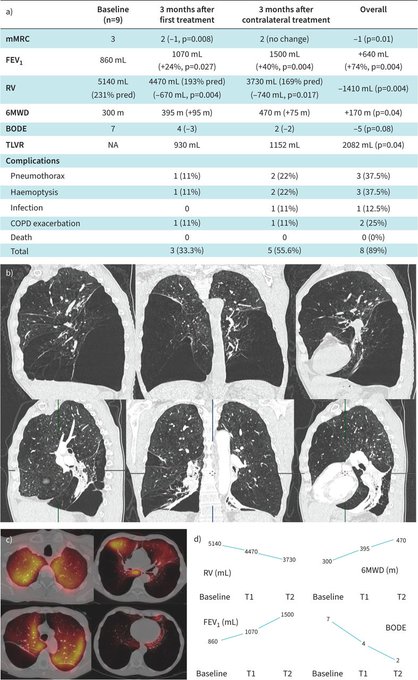
Early pulmonary rehabilitation shortly after
#AECOPD
leads to a faster recovery in physical performance than initiated in the stable phase. Adherence to rehabilitation is significantly higher when initiated shortly after an exacerbation.
0
51
87
Pneumomediastinum is more frequent in
#COVID19
patients with ARDS despite the use of a protective ventilatory approach. Lung frailty, and not barotrauma, appears to be the main cause of this finding.
0
39
87
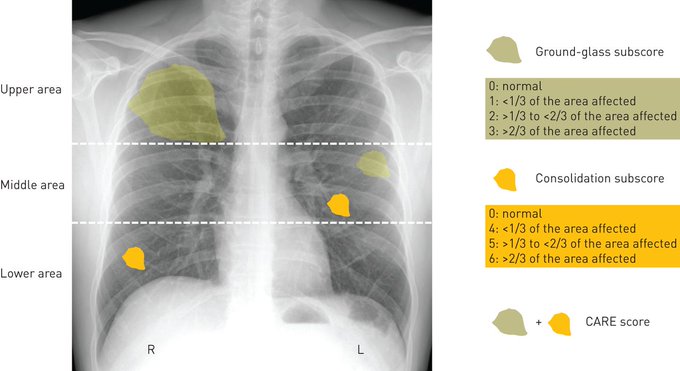
CARE is a reliable tool with a good prognostic performance to assess the severity of pulmonary involvement due to
#COVID19
0
40
79
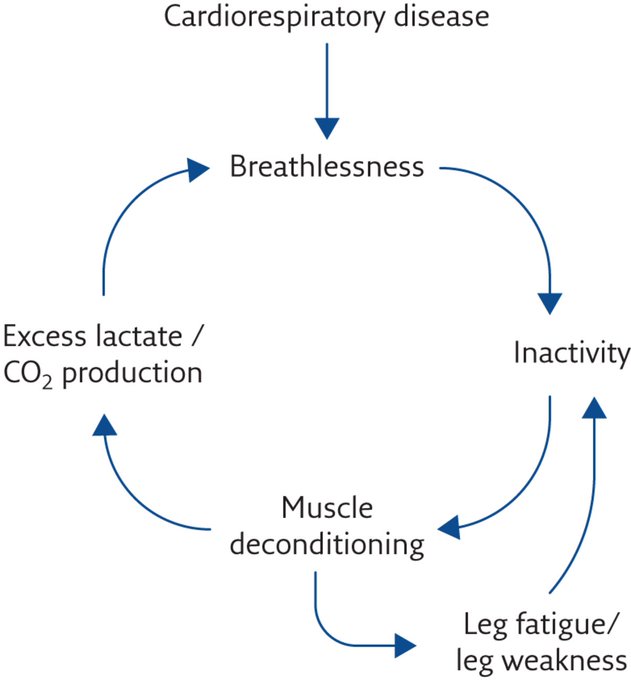
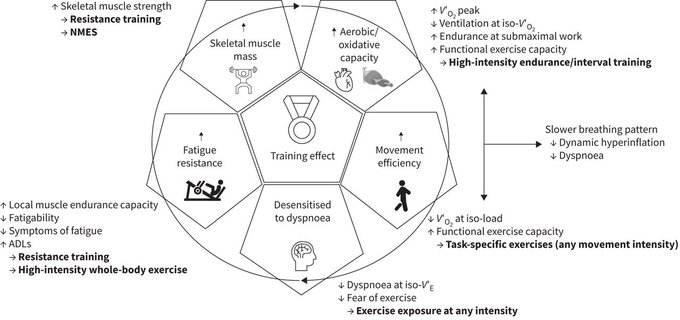
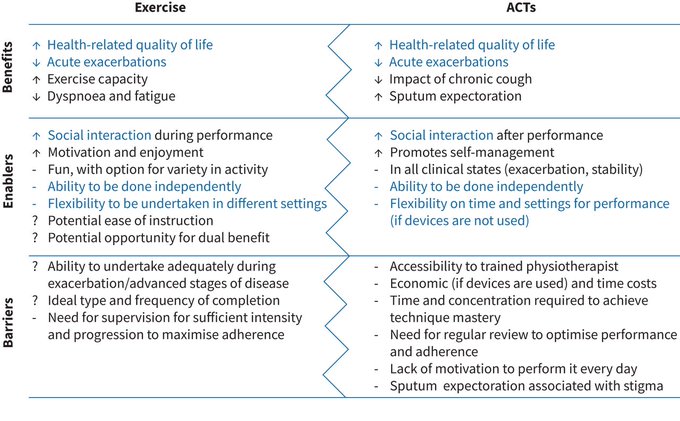
Dyspnoea and fatigue are common in chronic lung disease and are associated with decreased exercise capacity, muscle weakness and physical inactivity.
#pulmonaryrehab
is effective at targeting these extrapulmonary features, but is underused.
@burtin_chris
0
19
77
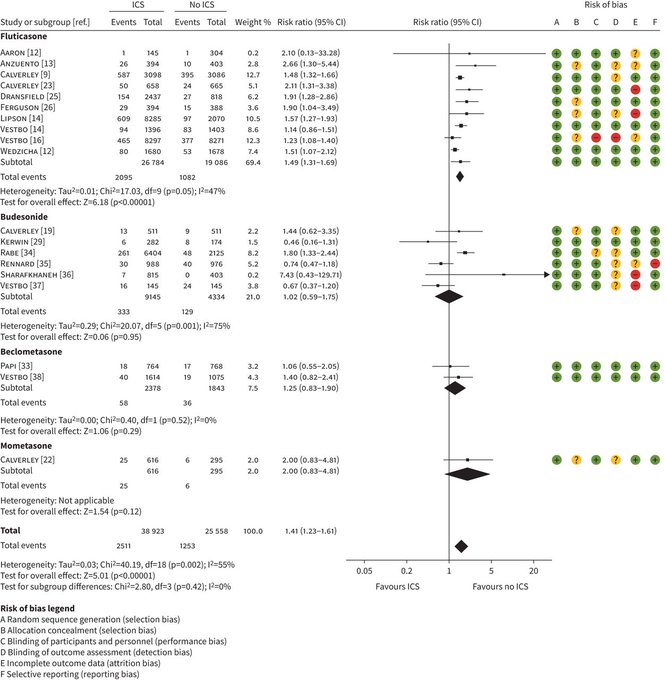
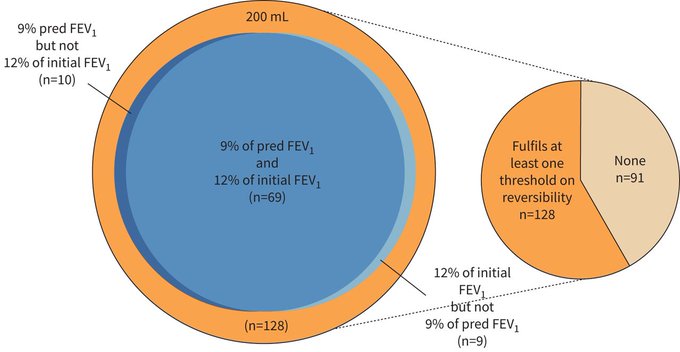
This
@EuroRespSoc
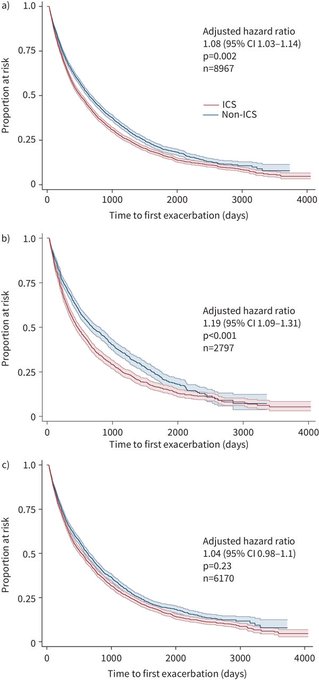
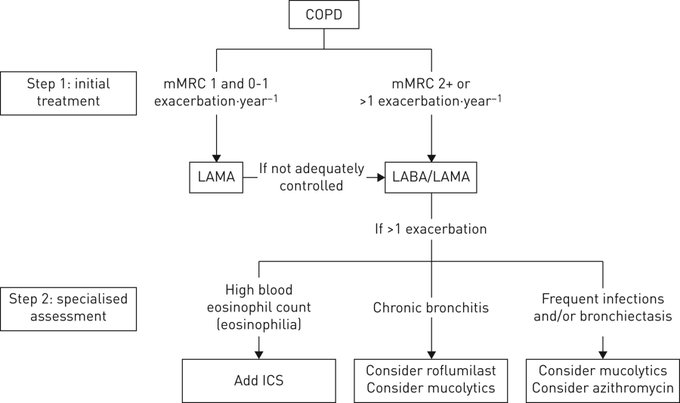
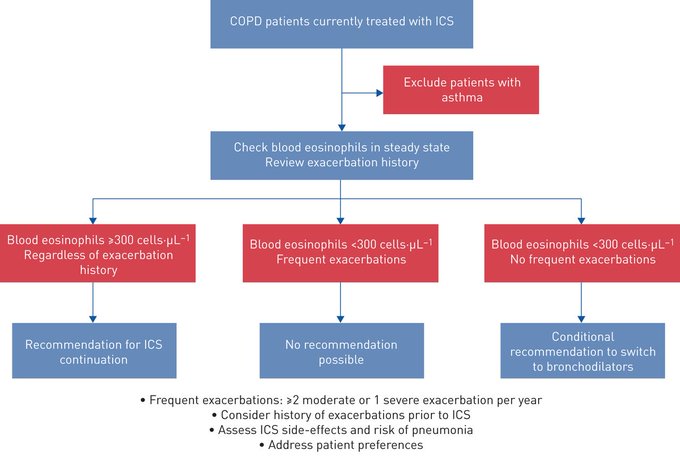
short guideline summarises the evidence and provides recommendations for ICS withdrawal in patients with COPD
3
48
78
CPAP can be successfully used in a number of
#COVID19
patients with hypoxaemic respiratory failure and gas exchange and radiological findings similar to those generally considered to be indications for invasive mechanical ventilation
0
45
79